COVID-19: A Guide to Symptoms & Treatment
I know you’re worried about the recent COVID-19 news, and I want you to take a deep breath. You’re reading the headlines, you’re seeing the numbers, and it’s natural to feel overwhelmed. However, I want to reassure you that as a medical community, we’ve learned so much since the early days. We understand the corona virus in humans far better now, and we have real, reliable tools to manage it.
Forget the panic you see online. My job right now is to cut through the noise and explain this whole thing to you clearly, compassionately, and professionally. We’re going to walk through this step-by-step, just like I do with all my patients.
What COVID-19 Really Is: An Unwelcome Guest
Think of the COVID-19 virus, which is the corona virus in humans, not as a massive invasion force, but as an unwelcome, microscopic party guest.
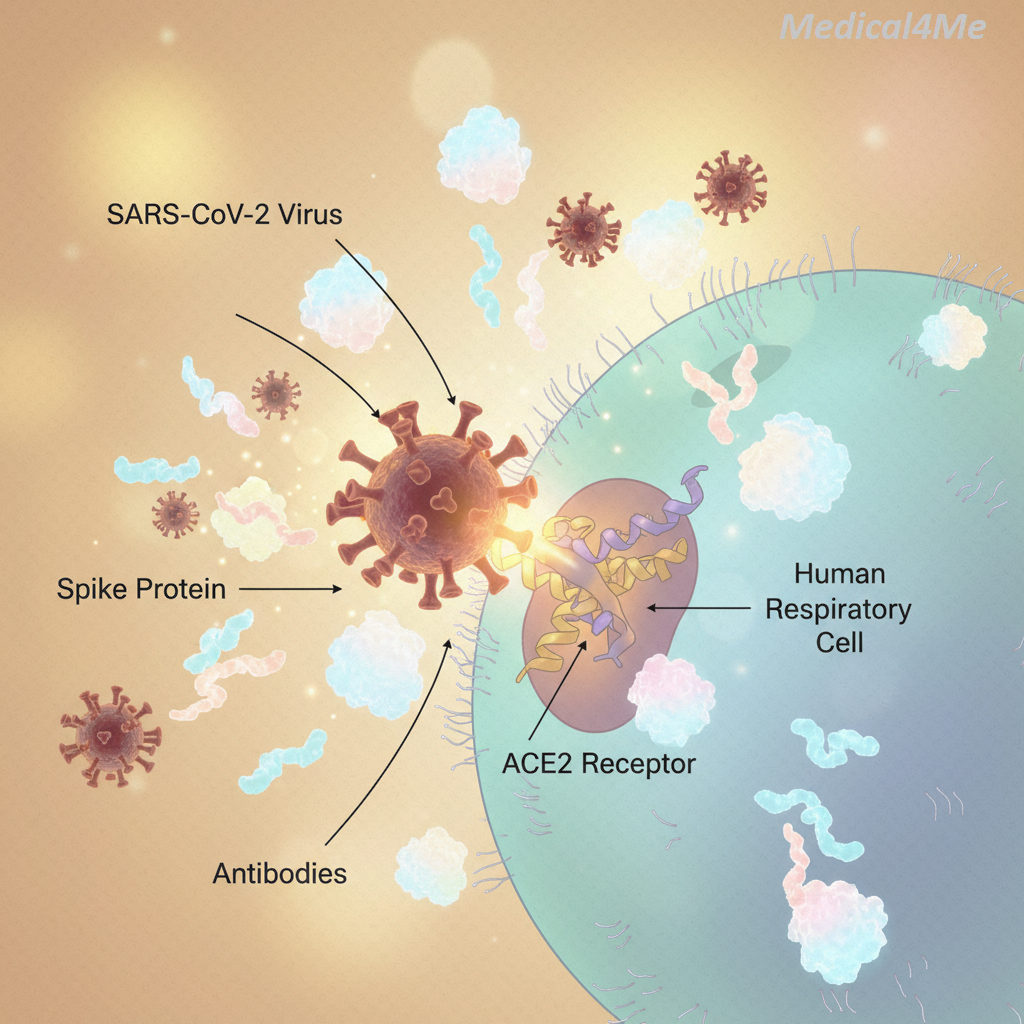
It’s an entirely new party you weren’t expecting. Here’s the analogy: Your body is a heavily protected neighborhood. The front door is your nose and mouth. This tiny viral particle, the COVID-19 virus, has a specific key—the spike protein—that unlocks the ACE2 receptor on your cells. This receptor is like the doorman. The virus sneaks in, locks the door, and immediately starts making copies of itself using your cell’s internal machinery, essentially turning your house into a virus-manufacturing plant.
Because of this, the initial symptoms you feel are simply your body’s police force, the immune system, rushing in to fight the uninvited guest and shut down the factory. This reaction is what causes fever, aches, and fatigue. It’s an exhausting battle, and unfortunately, sometimes that immune response can overdo it, leading to the complications we’ve seen in the lungs and other organs.
My first thought when a patient describes this is always to remind them that their body is already actively fighting this, and we’re just here to support its natural defenses.
Recognizing the Symptoms: When to Pay Attention
When the pandemic started, every cough felt like a crisis. However, we’ve now developed a clear profile for the symptoms caused by the corona virus in humans. Most people experience something similar to a bad cold or flu, but there are certain indicators that you shouldn’t ignore.
I was recently talking to a patient, Zoya, a 32-year-old software architect, who in February 2020 thought her fatigue was simply a severe flu. She called me at 6 PM one Tuesday, worried because she had a dry cough that felt different from anything she’d ever had. In addition, she mentioned a strange, dull headache. Since widespread testing wasn’t available yet, we could only treat the symptoms and advise strict isolation. Her case, like so many others then, was a frightening mystery that we simply monitored day by day.
Here is a quick checklist of the most common signs:
- Persistent fatigue that doesn’t improve with rest.
- Sudden onset of a new, dry cough.
- Fever or chills.
- Muscle aches or body pain.
- New loss of taste or smell—this is often a huge red flag.
- Sore throat or congestion.
- Gastrointestinal issues, like nausea or diarrhea.
The Problematic Progression
The tricky part about the corona virus in humans is that the illness can progress bafflingly fast in some cases. Usually, symptoms appear two to 14 days after exposure. Furthermore, while the initial symptoms might be mild, it’s that second week where we look for potential deterioration, especially in breathing.
Therefore, monitoring your oxygen levels, particularly if you have any pre-existing conditions like other conditions, is extremely important during this period.
Root Causes and Vulnerabilities
We know COVID-19 is caused by the SARS-CoV-2 virus, but the more interesting question is why it affects people so differently. To be perfectly honest, the medical community is still exploring the precise mechanism for why some individuals suffer WHO data shows severe, prolonged illness while others are asymptomatic.
The primary vulnerability involves underlying chronic conditions. *Age is a major risk factor*, simply because the immune system becomes less robust over time and is prone to over-reacting inflammatorily.
I had Farooq, a 68-year-old retired bookbinder, who had a history of well-managed diabetes. In April 2020, he acquired the virus from a limited community spread. Because of his diabetes, his body’s ability to regulate the inflammatory response was compromised. Consequently, when the virus hit, his immune system panicked, leading to widespread inflammation that threatened his lungs and heart. Back then, with no proven antiviral drugs available, all we could do was focus on supportive care and the careful, off-label use of anti-inflammatory medications to manage the cytokine storm—that over-reaction—he was experiencing. We faced immense challenges trying to keep him stable.
However, it’s not just age. Any condition that causes chronic inflammation, such as obesity, heart disease, or even autoimmune disorders, gives the virus a significant advantage. This is why we focus so heavily on vaccination and overall health maintenance.
The Diagnostic Journey: Finding Answers
When you’re feeling ill, getting a diagnosis is the first step toward reclaiming control. The diagnostic process for the corona virus in humans is straightforward now, but it still requires careful attention to timing and methodology.
I had a phone call from Shireen, a 55-year-old homemaker and grandmother. This was in January 2020, when the CDC was just starting to ramp up surveillance. She was anxious because she had been at a large gathering before travel restrictions were in place, but she felt perfectly fine. We needed to know if she was an asymptomatic carrier. At the time, testing was restricted to only those with severe symptoms and recent travel history to specific regions.
Here is the simple, numbered process we follow today:
- Symptom Review and Exposure History: We first discuss your timeline. When did you feel sick? When was your last exposure? This helps us determine the best day for testing, as testing too early can result in a false negative.
- The Gold Standard RT-PCR Test: This test is highly sensitive and is usually performed via a nasal swab. It detects the genetic material of the virus. We use this primarily for confirming active infection, and it remains the most reliable method, even if it’s uncomfortable.
- The Rapid Antigen Test: This can be done at home and provides quick results. It looks for viral proteins. While convenient, this test is less sensitive, particularly in the early or late stages of the infection. Therefore, a negative result may need confirmation with a PCR test if symptoms persist.
- Antibody Testing (Less Common): If you’ve been sick for a while and want to know if you’ve had the virus, an antibody test can confirm past infection. It looks for antibodies your body produced in response to the virus. Mayo Clinic explains that antibody tests aren’t used to diagnose current infection.
- Severity Assessment (If Positive): If your test is positive, we then assess your risk factors and symptom severity (checking oxygen saturation, lung sounds, and vital signs) to determine if you need outpatient management or immediate hospitalization.
The Treatment Reality: Strategies for Recovery
Lifestyle and Home Care
The vast majority of people manage the corona virus in humans effectively at home. In many ways, recovery involves doing the simple things well.
This is the non-negotiable foundation of treatment. You need strict rest, which means truly laying down and doing nothing. Hydration is also incredibly vital; you must drink plenty of fluids to thin out mucus and support kidney function. Using over-the-counter fever reducers, like acetaminophen or ibuprofen, can also help manage fever and body aches.
Medical Options for High-Risk Patients
For those who are high-risk or have moderate to severe illness, we have excellent, targeted medical options now. We’ve moved beyond the early, clumsy treatments into refined antiviral and anti-inflammatory therapies.
I often discuss two main types of medication with my patients:
1. Antiviral Medications (e.g., Paxlovid): This is typically a combination of nirmatrelvir and ritonavir, prescribed within five days of symptom onset. This drug works by inhibiting an enzyme the virus needs to replicate itself. In short, it slams the brakes on the viral manufacturing plant. While effective in preventing severe outcomes, it can have side effects like a temporary metallic taste in the mouth (known as the “Paxlovid mouth”) and potential drug interactions, especially with heart medications.
2. Anti-inflammatory Treatments (e.g., Dexamethasone): This is a powerful steroid. It’s not used to fight the virus itself, but rather to calm the severe, damaging over-reaction of the immune system (the cytokine storm) in hospitalized patients. It reduces inflammation rapidly. However, its use is carefully managed because side effects can include elevated blood sugar and mood changes.
This is a comparison of the general approaches we use here at Medical4Me:
| Treatment Type | Pros | Cons |
|---|---|---|
| Outpatient Antivirals | Reduces the chance of hospitalization significantly; quick recovery time; easy oral administration. | Must be started early (within 5 days); significant potential for drug interactions; metallic taste side effect. |
| Inpatient Anti-inflammatories | Dramatically lowers the risk of death in hospitalized patients; calms the hyper-inflammatory immune response fast. | Only used in severe cases; potential for serious side effects like high blood sugar or infection risk; requires hospitalization. |

Navigating Long COVID: A Baffling Challenge
The phenomenon of Long COVID, where symptoms persist for weeks or months after the initial infection, remains a frustrating challenge. It’s like the unwelcome guest left, but their mess is still clogging up your system.
Symptoms often include chronic fatigue, difficulty concentrating (brain fog), and persistent shortness of breath. We’re still learning about this, but the working theory is that it involves either residual viral particles, micro-clotting, or persistent, low-grade inflammation.
I mentioned in recent posts that approaching Long COVID requires immense patience and a multidisciplinary team.
When to Get Emergency Help
While you don’t need to panic, you do need to be prepared. If you’re managing COVID-19 at home, please watch for these signs. They signal that the immune battle is becoming overwhelming and you need immediate professional support.
Urgent Red Flags
- Difficulty breathing or shortness of breath that worsens when you move.
- Persistent pain or pressure in the chest.
- New confusion or an inability to wake or stay awake.
- Pale, gray, or blue-colored skin, lips, or nail beds—this indicates poor oxygen levels.
- Inability to tolerate any fluids for more than 24 hours.
If you observe any of these symptoms, please don’t wait. Seek emergency medical care immediately.
Common Questions I Hear in Clinic
They share many symptoms, including fever and aches, which can be confusing. However, COVID-19 is much more likely to cause loss of taste/smell and can lead to more severe, specific lung damage. Testing is the only way to know for sure.
Absolutely. CDC guidelines state that the vaccine boosters are the single best way to reduce your risk of severe disease, hospitalization, and death from the circulating variants. Protection wanes over time, so staying updated is key.
While studies are mixed, we do know that low Vitamin D levels are associated with a higher risk of severe outcomes. I generally recommend ensuring adequate Vitamin D levels, as it supports overall immune health, but it’s not a cure.
Yes, you definitely can. Immunity from natural infection doesn’t last forever and isn’t always robust against new variants. You should still consider vaccination and follow preventative measures, even after recovering from a previous infection.
No, it’s generally not. Excessive exertion during the acute phase or recovery can potentially lead to myocarditis (inflammation of the heart muscle). Listen to your body and ease back into physical activity very slowly and cautiously only after you feel completely recovered.
My Final Professional Advice
Please remember this: fear and stress do not help your immune system. Knowledge and preparation do. We have powerful, effective ways to handle the corona virus in humans now, and your proactive approach—staying informed, getting vaccinated, and prioritizing your overall health—is your best defense.
Take care of yourself, pay attention to those red flags, and don’t hesitate to call if you have any concerns. We’re in this together, and we’re ready to help you navigate it with confidence and calm.


💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.