Crohn’s Disease: A Guide to Symptoms & New Treatments
I understand this can be scary. You’re likely here because you or a loved one is grappling with chronic digestive issues, and the fear of a diagnosis like Crohn’s Disease is overwhelming. The truth is, facing this inflammatory bowel disease (IBD) is a challenge, and it’s completely normal to feel frustrated or isolated. According to the CDC, approximately 3.1 million adults in the U.S. have been diagnosed with an IBD, showing just how common this chronic inflammatory disease actually is.
But look, I want you to know that modern management has revolutionized life for patients. This article isn’t about dread; it’s about empowerment. We’re going to break down exactly what Crohn’s Disease is, why it happens, and how the latest, most effective therapy—like biologics—can genuinely restore your quality of life. As a medical professional, I’ve seen patients reclaim their lives, and you can too. We will cover the specific signs and latest treatment options, ensuring you feel informed and ready to take control of your health care journey. We’ll start with the basics.
What is Crohn’s Disease? The Plumbing and Fire Analogy
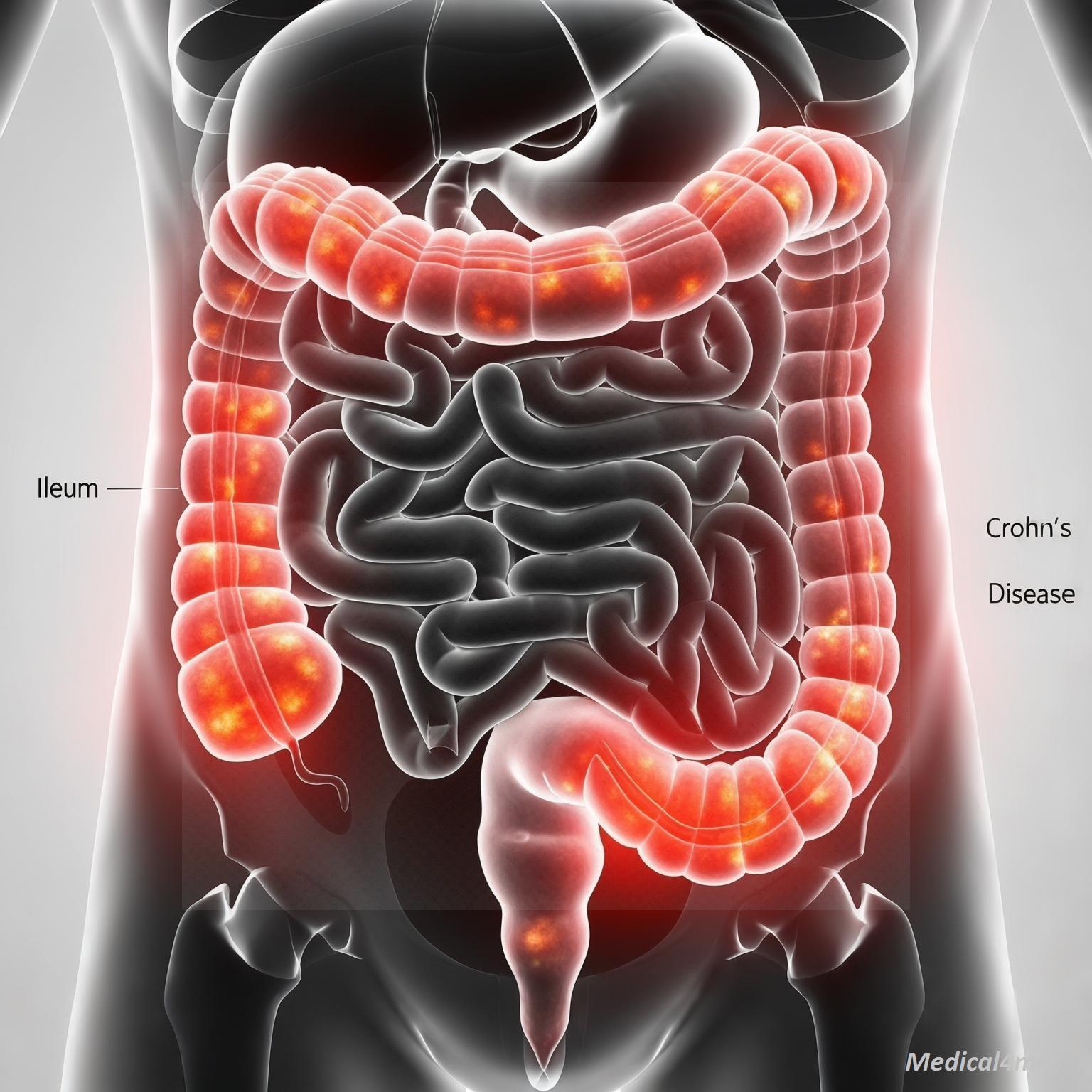
Here’s the thing: people often confuse Crohn’s Disease with generic digestive issues like IBS. But it’s much more specific. To keep it simple, think of your digestive tract as a long stretch of flexible plumbing, from your mouth to your anus. This chronic inflammatory disease is basically a deep, patchy fire that can break out anywhere along that plumbing, usually deep in the intestinal wall.
The Official Definition
Crohn’s Disease is a type of inflammatory bowel disease (IBD) characterized by chronic inflammation of the gastrointestinal (GI) tract. Unlike Ulcerative Colitis, which affects only the colon’s lining, Crohn’s inflammation is *transmural*, meaning it goes through all layers of the bowel wall, and it can occur in patches (called skip lesions) throughout the GI tract, though it most often affects the terminal ileum (the end of the small intestine).
This deep, patchy inflammation is what causes the long-term signs. When the intestinal wall swells, it can’t absorb nutrients properly. It restricts the pathway, causing pain, blockages, and often leading to malabsorption. In my clinical experience, it’s the severity of this gut inflammation and its location that dictates the specific symptoms a patient experiences. It’s a progressive disease that needs consistent management to prevent long-term damage.
Recognizing Symptoms and Signs of Gut Inflammation
The early indicators of IBD can be confusing, often mimicking less serious conditions. But with Crohn’s Disease, the symptoms persist and worsen. It helps to categorize them for better diagnosis.
The Most Common Indicators
- Persistent Diarrhea: This is often the most relentless sign. The inflammation prevents proper water absorption, leading to frequent, watery stools.
- Abdominal Pain and Cramping: This is classic, often centered in the lower right abdomen, and gets worse after eating.
- Weight Loss and Malnutrition: Your inflamed intestines can’t absorb vitamins, minerals, or fats well, causing unexplained weight loss.
- Fatigue: Chronic inflammation uses massive amounts of energy, leaving you absolutely drained.
And actually, because it’s a systemic immune disorder, the signs can show up outside the GI tract. We call these extra-intestinal manifestations. These include arthritis (joint pain), eye inflammation, and skin rashes. It’s a full-body illness, not just a gut problem. Well, recognizing these indicators early is key to successful long-term management.
Quick Self-Check Guide: Severity Levels
🟢 Mild: Intermittent diarrhea (4-5 times/day), mild abdominal tenderness, slight weight loss, no fever. You’re still functional, but you know something’s wrong. This stage is often responsive to less aggressive treatment.
🟡 Moderate: Frequent diarrhea (6-8 times/day), significant pain not controlled by over-the-counter medicine, fever, and noticeable weight loss. Your daily routine is compromised. This requires aggressive therapy to achieve mucosal healing.
🔴 Severe: Constant, debilitating diarrhea (10+ times/day, potentially bloody), high fever, severe abdominal guarding, significant weight loss (over 10%), and complications like abscesses. This needs immediate medical attention.
Understanding Causes and Risk Factors for Crohn’s Disease
Many patients ask me, “Doctor, what caused this?” I always tell them this: You didn’t do anything wrong. Crohn’s Disease isn’t caused by a stressful job or a poor diet. It’s the result of an inappropriate and sustained immune response, but we don’t know the exact trigger.
However, we do know the key risk factors that make a person susceptible to this inflammatory bowel disease:
- Genetics (The Family Link): Genetics play a major part. If you have a first-degree relative—a parent or sibling—with IBD, your risk is significantly higher. Specific genes, like *NOD2*, are strongly associated with the disease.
- Smoking (The Biggest Enemy): Honestly, smoking is the single most powerful, *controllable* risk factor. Smokers are twice as likely to develop Crohn’s Disease as non-smokers. Once diagnosed, smoking makes flare-ups more frequent and severe, often requiring surgery.
- Location and Environment: The incidence is highest in industrialized countries and urban areas, particularly North America and Northern Europe. This suggests that diet, pollution, or the “hygiene hypothesis” might alter the gut microbiome and trigger the inappropriate immune response.
- Antibiotics and NSAIDs (Potential Triggers): While not direct causes, frequent use of broad-spectrum antibiotics or NSAIDs (like Ibuprofen) can severely disrupt the delicate balance of the gut flora and increase gut permeability, potentially triggering a flare.
What I’ve learned is that it’s usually a perfect storm—a genetic predisposition combined with an environmental trigger that essentially confuses your immune system. It mistakenly attacks the harmless bacteria and food particles in your digestive system, leading to the chronic gut inflammation that defines Crohn’s Disease.
The Diagnostic Journey: Taking the Right Steps
Getting a proper diagnosis of IBD can be a frustrating journey, and you’re not alone if it takes time. Why? Because the initial signs mimic so many other conditions. But let’s look at the step-by-step process a medical professional uses to confirm this diagnosis and rule out others.
What to Expect During Diagnosis
1. The Initial Conversation and Physical Exam: We start here. I need to know the pattern of your pain, frequency of bowel movements, and whether you’ve lost weight. A physical exam often includes checking for tenderness and signs of anal involvement, which are common with Crohn’s Disease.
2. Blood Tests and Stool Samples: Simple blood tests give us huge clues. We check for anemia and elevated inflammation markers, such as C-Reactive Protein (CRP) and Erythrocyte Sedimentation Rate (ESR). We also check stool samples to rule out infections, which can mimic a flare. Calprotectin in the stool is a very useful non-invasive test for gut inflammation.
3. Endoscopy and Colonoscopy: These are the gold standards. A colonoscopy allows the doctor to visually inspect the colon and the terminal ileum (where regional enteritis often starts). During the procedure, small tissue samples (biopsies) are taken. Finding “skip lesions” (patches of inflammation) and deep ulcers helps confirm this specific inflammatory bowel disease.
4. Imaging Studies (CT, MRI, Capsule Endoscopy): Sometimes, the inflammation is deep in the small intestine, out of reach of a standard scope. We might use an MRI or a CT scan to look for strictures (narrowing) or abscesses. A capsule endoscopy—swallowing a tiny camera—can image the entire small bowel. According to Mayo Clinic researchers, a detailed assessment and use of multiple diagnostic tools are necessary because Crohn’s has such a varied presentation.
Treatment Options Comparison: Finding Your Management Plan
The main goal of Crohn’s Disease therapy isn’t just to make you feel better—it’s to achieve mucosal healing, meaning the inflammation in the intestinal lining actually goes away. We use medicine to suppress the misguided immune response. The strategy is typically stepped, moving from older drugs to advanced ones as needed. It’s a personalized treatment plan.
Mainstay Medications for Gut Inflammation
| Treatment Class | Primary Action | Use Case & Effectiveness | Key Side Effects |
|---|---|---|---|
| Aminosalicylates (5-ASAs) | Targets inflammation in the bowel lining. | Mild symptoms or maintaining remission (less effective for Crohn’s than UC). | Nausea, headache, mild abdominal pain. |
| Corticosteroids (Prednisone) | Powerful, broad-spectrum anti-inflammatory. | Used short-term to quickly suppress severe flare-ups (to induce remission). | Serious long-term effects: bone thinning, weight gain, mood swings. |
| Immunomodulators (Methotrexate, Azathioprine) | Broadly calms the immune system to reduce inflammation. | Used for moderate-to-severe disease to help maintain long-term remission. | Higher infection risk, liver toxicity monitoring required. |
| Biologics (Infliximab, Adalimumab) | Target specific inflammatory proteins (e.g., TNF-alpha). | Standard for moderate-to-severe Crohn’s Disease; highly effective in achieving mucosal healing. | Infusion reactions, increased risk of serious infection (tuberculosis screening required). |
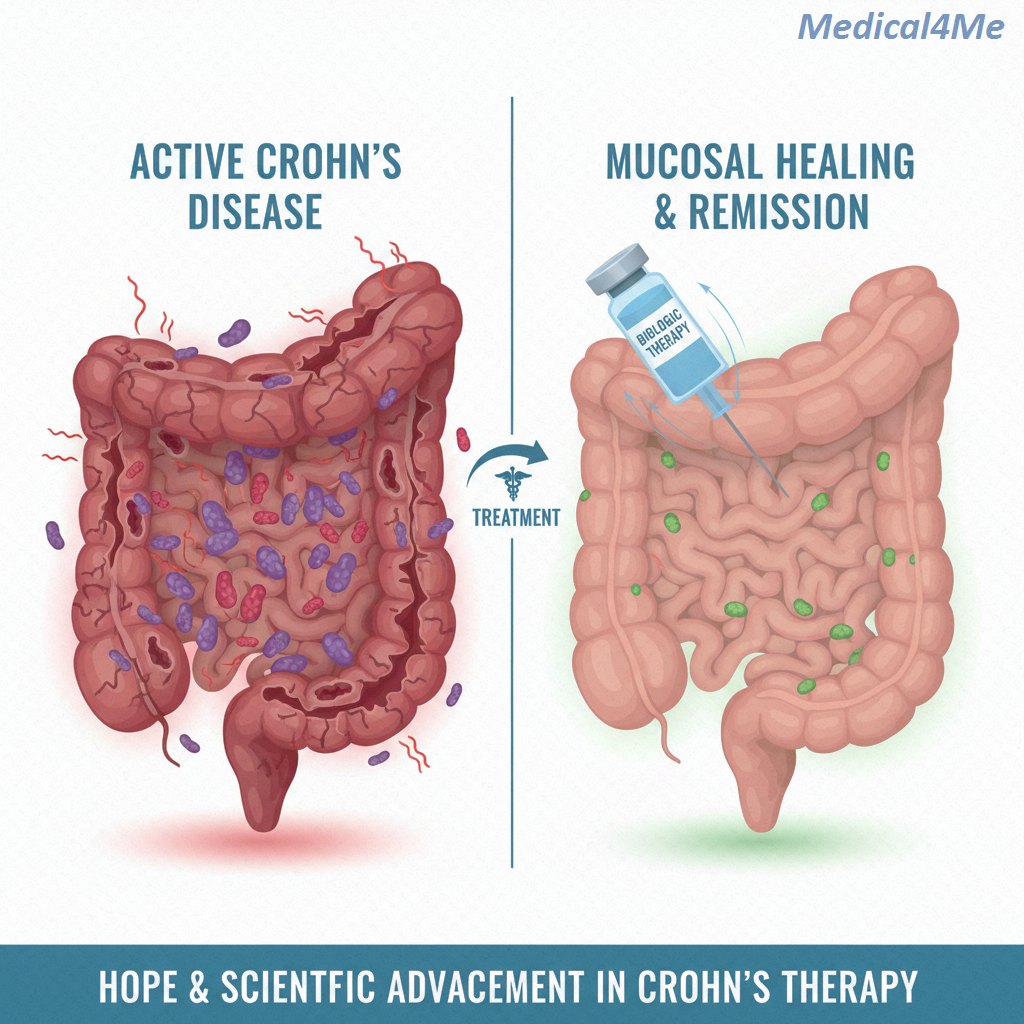
The truth is, Biologics have revolutionized the management of this inflammatory bowel disease. They are now the preferred initial therapy for patients with moderate-to-severe disease due to their high efficacy in achieving long-term, steroid-free remission. But they are costly, and they require careful monitoring by a medical professional. We always personalize your management plan based on disease severity and location, aiming for deep and lasting mucosal healing.
Prevention Strategies: Taking Control of Your Health
Since we can’t truly prevent the initial onset of Crohn’s Disease due to the genetic component, prevention focuses entirely on preventing flare-ups and managing the long-term risk of complications. Prevention is basically the lifestyle foundation that supports your medicine.
Daily and Weekly Action Items for Prevention
- Daily: If you smoke, you need to quit. This is the single most important lifestyle modification you can make. It impacts every aspect of your gut inflammation. Consult your doctor immediately about cessation programs.
- Weekly: Engage in low-impact exercise, like walking or yoga, for at least 150 minutes. It reduces stress, which we know can trigger flare-ups.
- Dietary Control: Keep a detailed food diary to identify your personal trigger foods (dairy, high-fiber, or fatty foods often cause trouble) and strictly avoid them. This is complementary to your treatment.
- Medication Compliance: Seriously, don’t miss doses. This is the main reason patients slide out of remission. Immunomodulators and biologics need to be taken exactly as prescribed.
- Screenings: You’re at a higher risk of colorectal cancer, so regular surveillance colonoscopies (usually every 1 to 2 years after 8 years of diagnosis) are mandatory. According to CDC guidelines, proactive screening is vital for long-term health care.
And, you know, stress management can’t be overstated. Stress won’t *cause* Crohn’s Disease, but it certainly triggers flares by increasing inflammation system-wide. Practicing mindfulness or deep breathing is as important as taking your drug.
Latest Research & Developments: Hope on the Horizon
This is where things get genuinely exciting for patients with gut inflammation. Research has progressed incredibly fast, especially in the last few years. It gives us real hope for better management.
1. JAK Inhibitors (Small Molecule Drugs): A major breakthrough has been the introduction of Janus Kinase (JAK) inhibitors (like upadacitinib) in 2023. These are small molecule drugs you can take orally, unlike biologics, which require injections or infusions. Research published in *The New England Journal of Medicine* showed high rates of clinical remission in patients who had failed prior biologic treatment. This is huge news, offering new therapy for those who haven’t responded well to standard medicine.
2. Personalized Medicine via Biologic Drug Monitoring: Now, physicians are moving toward therapeutic drug monitoring (TDM). Researchers at the Cleveland Clinic have pioneered methods to measure the actual drug levels of biologics in a patient’s blood and adjust the dosage to optimize the immune response. This ensures the patient gets the maximum effect, reducing the chance of the drug failing later on. This precision health care approach is the future of IBD management.
3. Targeted Anti-Integrin Therapy: New monoclonal antibodies are being developed that specifically block white blood cells from entering the inflamed gut tissue. These anti-integrin drugs are highly targeted for gut inflammation and show promise in achieving high rates of mucosal healing without the broad systemic effects of older medicine. They’re becoming a critical part of the modern treatment arsenal for Crohn’s Disease.
When to Seek Medical Help: The Red Flags You Must Know
Look, I want you to feel empowered, but I also need you to be vigilant. If you are a known Crohn’s Disease patient, a flare-up is one thing, but an emergency is another. You must know the difference.
⚠️ Emergency Red Flags: Call 911 or Go to the ER Now
If you experience any of the following signs, do not wait. This is a medical emergency that requires immediate attention from a medical professional:
- Fever over 101°F (38.3°C): A persistent high temperature can signal a serious infection, like an abscess, which needs drainage and antibiotics right away.
- Severe, Unrelenting Abdominal Pain: Pain so bad you can’t stand up, or that is accompanied by nausea and vomiting, could mean an intestinal blockage (stricture) or perforation.
- Massive Rectal Bleeding: Passing large amounts of bright red blood. While mild blood is common with gut inflammation, heavy bleeding is an emergency.
- Signs of Dehydration: Inability to keep fluids down, extreme dizziness, dark urine, or extreme weakness.
If you feel symptoms are rapidly worsening or you’re unable to tolerate food or fluids, please, find help right away. Timely intervention can often prevent the need for emergency surgery and manage this chronic inflammatory disease.
Overcoming the Fear of the Diagnosis
I’ve seen patients who have spent years chasing a proper diagnosis. I saw Elias, a 28-year-old student, just a few months ago. He’d spent eighteen months being told his chronic diarrhea, crushing fatigue, and 20-pound weight loss were “just stress.” He finally came to see me, exhausted and frankly, defeated. The diagnosis was moderate-to-severe Crohn’s Disease, mostly concentrated in his small intestine (terminal ileitis).
Elias was devastated. He pictured a life of endless bathroom trips and pain. But we started his personalized treatment plan with a biologic drug, and he committed to managing his stress. Within four months, his CRP dropped from 65 to 5, and his gut inflammation went quiet. Now, he’s back on the rugby field, studying for his exams, and living a full life. He still manages his IBD, of course, but the chronic inflammatory disease doesn’t manage him anymore. His story is what gives me hope for every patient.
Frequently Asked Questions My Patients Ask
Your Questions About Crohn’s Disease Answered
Crohn’s Disease is a chronic, lifelong inflammatory disease with no known cure yet. However, it’s highly manageable with modern medicine and lifestyle changes. The goal of management is to achieve and maintain ‘remission,’ where you have few to no signs, and the inflammation is gone (mucosal healing).
Neither diet nor stress *causes* Crohn’s Disease, but both can significantly trigger flare-ups. Stress affects the gut-brain axis, worsening symptoms. Diet helps by identifying and eliminating specific foods (like high-FODMAP items or fatty foods) that irritate an already inflamed intestine. Always talk to a medical professional before changing your diet.
Biologics are a class of advanced drugs (like Infliximab or Adalimumab) derived from living organisms. They specifically target and block key inflammatory proteins (like TNF-alpha) that cause gut inflammation. They are a breakthrough because they promote deep mucosal healing, leading to long-term remission, and they’re more effective than older, less-targeted drugs.
Yes, but planning is key. The best time to conceive is when your disease is in deep remission. Active Crohn’s flare-ups can increase risks for both mother and baby. You must work closely with your gastroenterologist and OB-GYN to ensure your drug regimen is safe and your nutritional status is optimal throughout the pregnancy.
Surgery is usually reserved for treating complications, not for ‘curing’ the condition itself. It’s often necessary to remove sections of the bowel that have developed strictures (narrowing), abscesses, or fistulas (abnormal connections) that aren’t responding to medicine. About 70% of patients will need surgery at some point.
The Path to Remission: Taking the Next Step
So, we’ve walked through the complexity of Crohn’s Disease, from its sometimes-confusing symptoms to the cutting-edge treatment options like biologics and JAK inhibitors. The key takeaway is simple: this is a manageable disease. Your goal should be to partner with your physician to achieve deep mucosal healing, not just symptom relief. Don’t settle for “good enough” when it comes to your health care.
Here are your next actionable steps:
- Seek Specialized Care: If you suspect IBD, see a gastroenterologist immediately. Early diagnosis changes everything.
- Embrace Compliance: Stick to your prescribed medicine. Consistency prevents devastating flare-ups.
- Prioritize Wellness: Implement the stress management and dietary prevention tips we discussed.
Remember Elias. You have the power, with the right therapy, to put this chronic inflammatory disease firmly in its place. Take the first step today and reclaim your future.

💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.