Dementia: A Guide to Causes & New Hope
I understand this can be scary. You’re likely searching for answers because you’ve noticed a small, worrying change in yourself or a loved one—a repeated question, a missed appointment, a struggle with once-simple tasks. The shadow of Dementia is something many people feel overwhelmed by. But look, I want you to know you aren’t alone in this fear, and knowledge is the first step toward taking control.
The global reality is stark: WHO data shows over 55 million people worldwide live with Dementia, and a new case is diagnosed every three seconds. That statistic is massive, but it also means an immense amount of research is focused on this challenge. This article is your empathetic guide, written not just by a medical professional but by someone who understands the weight of a diagnosis. We’ll break down the warning signs, explore the different types, discuss current treatment options, and focus on the latest research that offers real hope for future management of cognitive decline. We’ll start by defining exactly what we are facing.
What is Dementia? The Clouding of the Mind’s Lens
Here’s the thing: many people mistakenly think Dementia is a specific disease, like with other conditions. Actually, it’s basically an umbrella term, a collection of symptoms that involve serious memory loss and a severe decline in at least two other cognitive functions, such as language, problem-solving, or the ability to focus. These indicators must be severe enough to interfere with daily life and independence.
The Clinical Definition
Dementia is defined as a persistent and progressive decline in cognitive function—memory, thinking, and reasoning—caused by damage to brain cells, typically due to a neurodegenerative condition like Alzheimer’s disease. This mental decline is fundamentally different from the occasional forgetfulness that comes with normal aging.
Think of the mind like a complex library. Mild aging might mean you misplace a book occasionally. Dementia, however, means the cataloging system is breaking down, shelves are collapsing, and you can’t locate the information you know is there. The most common cause of Dementia is Alzheimer’s disease, responsible for 60-80% of cases. But other specific conditions, like Vascular Dementia and Lewy Body Dementia, also fall under this umbrella. Well, identifying the specific underlying cause is absolutely essential for the right management.
Recognizing Symptoms and Signs of Cognitive Decline
The earliest symptoms of Dementia can be subtle, and often, family members dismiss them as normal aging. But what I’ve learned is that it’s the persistence and progression of these changes that should trigger a conversation with a physician. It’s not just forgetting a name; it’s forgetting how to operate a familiar appliance or getting lost on a well-known route. Let me explain the progression.
The Most Common Indicators
- Memory Loss that Disrupts Life: Forgetting recently learned information, or asking the same question over and over.
- Difficulty with Planning or Solving Problems: Struggling to follow a recipe or manage monthly bills.
- Confusion with Time or Place: Losing track of dates, seasons, or where they are.
- New Problems with Words (Speaking or Writing): Stopping mid-sentence or repeating themselves often.
- Poor Judgment: Giving away large sums of money or neglecting personal hygiene.
We use a simple framework to assess the severity:
Severity Check: From Mild to Major Neurocognitive Disorder
🟢 Mild Cognitive Impairment (MCI): Forgetfulness is noticeable to others but does not significantly affect independence or daily activities. They are still able to live alone and manage life, but a cognitive assessment is needed.
🟡 Mild Dementia: Clear symptoms of cognitive decline begin to affect daily living. Trouble with complex tasks (driving, finances). They need some assistance, but still manage basic self-care. This is where most treatment begins.
🔴 Major Neurocognitive Disorder: Significant memory loss and reasoning failure. Requires full-time assistance with daily life, including dressing, feeding, and hygiene. This stage demands extensive caregiver support.
And you know, early detection doesn’t change the ultimate diagnosis, but it absolutely changes the quality and efficacy of early management. Early diagnosis gives patients time to plan their future health care and allows medicine to have its best chance at slowing the progression, a sentiment I mentioned in recent posts about proactive care.
Understanding Causes and Risk Factors for Dementia
When a doctor confirms a Dementia diagnosis, the next crucial step is determining the cause. It’s not a single illness but many diseases that damage brain cells. Targeting the specific neurodegenerative condition allows for more focused therapy.
Primary Types and Underlying Causes
- Alzheimer’s Disease (Most Common): Caused by the abnormal buildup of proteins—amyloid plaques and tau tangles—that destroy brain cells. This leads to shrinking of the brain tissue, particularly in areas responsible for memory loss.
- Vascular Dementia (Second Most Common): Caused by damaged blood vessels in the brain, often following a stroke or multiple small strokes. This is why managing high blood pressure and cholesterol is vital for brain health.
- Lewy Body Dementia (LBD): Caused by abnormal protein deposits (Lewy bodies) in the brain that affect thinking, memory loss, and movement control. Symptoms often include visual hallucinations.
- Frontotemporal Dementia (FTD): Affects the frontal and temporal lobes, areas associated with personality, behavior, and language. Symptoms often appear much earlier (45-65 years old) than Alzheimer’s.
Key Risk Factors You Can Influence
What I’ve learned is that roughly 40% of Dementia cases may be preventable by addressing modifiable risk factors. CDC guidelines state nine key risk factors account for a significant portion of preventable cases. These include less education, hearing loss, hypertension, obesity, smoking, depression, physical inactivity, social isolation, and diabetes. But it’s not all doom and gloom; managing these can dramatically reduce your long-term risk of developing cognitive decline.
The truth is, managing your heart is managing your brain health. If a heart is pumping efficiently and clean blood reaches the brain, the chance of vascular dementia drops significantly. This highlights why overall health care is so interconnected.
The Diagnostic Journey: Seeking Clarity and Peace of Mind
Getting a definitive diagnosis is probably the most emotionally draining part of the whole journey. I won’t lie; it takes time, patience, and a skilled medical professional. But it’s essential to rule out treatable conditions that mimic Dementia symptoms.
Step-by-Step Cognitive Assessment
1. Clinical History and Review: The doctor will spend a lot of time talking to you and a close family member. We need to know when the symptoms started and how they’re affecting daily life. We’ll also check your complete medicine list, because some drugs and even vitamin deficiencies can cause temporary confusion. That’s a huge relief when it happens.
2. Physical and Neurological Exam: This tests balance, reflexes, and coordination. It helps differentiate between conditions like Parkinson’s disease and LBD. We’re basically checking the hardware.
3. Cognitive and Neuropsychological Tests: This involves simple in-office tests like the Mini-Mental State Exam (MMSE) or the Montreal Cognitive Assessment (MoCA). These quantify the severity of the mental decline in areas like orientation, attention, and memory loss.
4. Brain Imaging (MRI/CT/PET): An MRI or CT scan is mandatory to rule out structural causes like tumors, strokes, or fluid buildup (hydrocephalus). A PET scan can sometimes be used in specialist centers to look for the presence of amyloid plaques, helping to confirm Alzheimer’s as the specific neurodegenerative condition causing the Dementia. This whole process is thorough by necessity, ensuring the right treatment path is chosen.
Treatment Options Comparison: Managing Dementia and Maintaining Quality of Life
Now, while we still don’t have a cure for most types of Dementia, we have effective therapy options that can manage symptoms and slow progression. The goal of all treatment is to maintain function and quality of life for as long as possible. Let’s look at the main types of medicine used.
Mainstay Medications for Cognitive Management
| Treatment Class | Examples | Primary Action | Use Case & Effectiveness |
|---|---|---|---|
| Cholinesterase Inhibitors | Donepezil, Rivastigmine | Boosts levels of acetylcholine, a chemical messenger vital for memory and judgment. | Used for mild to moderate Alzheimer’s and LBD. Improves cognitive function in some patients for a limited time. |
| NMDA Receptor Antagonist | Memantine | Regulates glutamate activity, another brain chemical. | Used for moderate to severe Alzheimer’s. Can improve daily function and behavior symptoms. Often used in combination with cholinesterase inhibitors. |
| Aducanumab/Lecanemab (Biologics) | Aducanumab, Lecanemab | Monoclonal antibodies that target and clear amyloid plaques. | New therapy for early Alzheimer’s. The first drugs to target the underlying cause, but they carry risks and require strict monitoring. |
| Non-Drug Interventions | Music therapy, Reminiscence, Exercise | Maintains cognitive engagement and improves mood/behavior. | Essential management for all stages. Reduces anxiety and dependence on medicine for behavioral issues. |
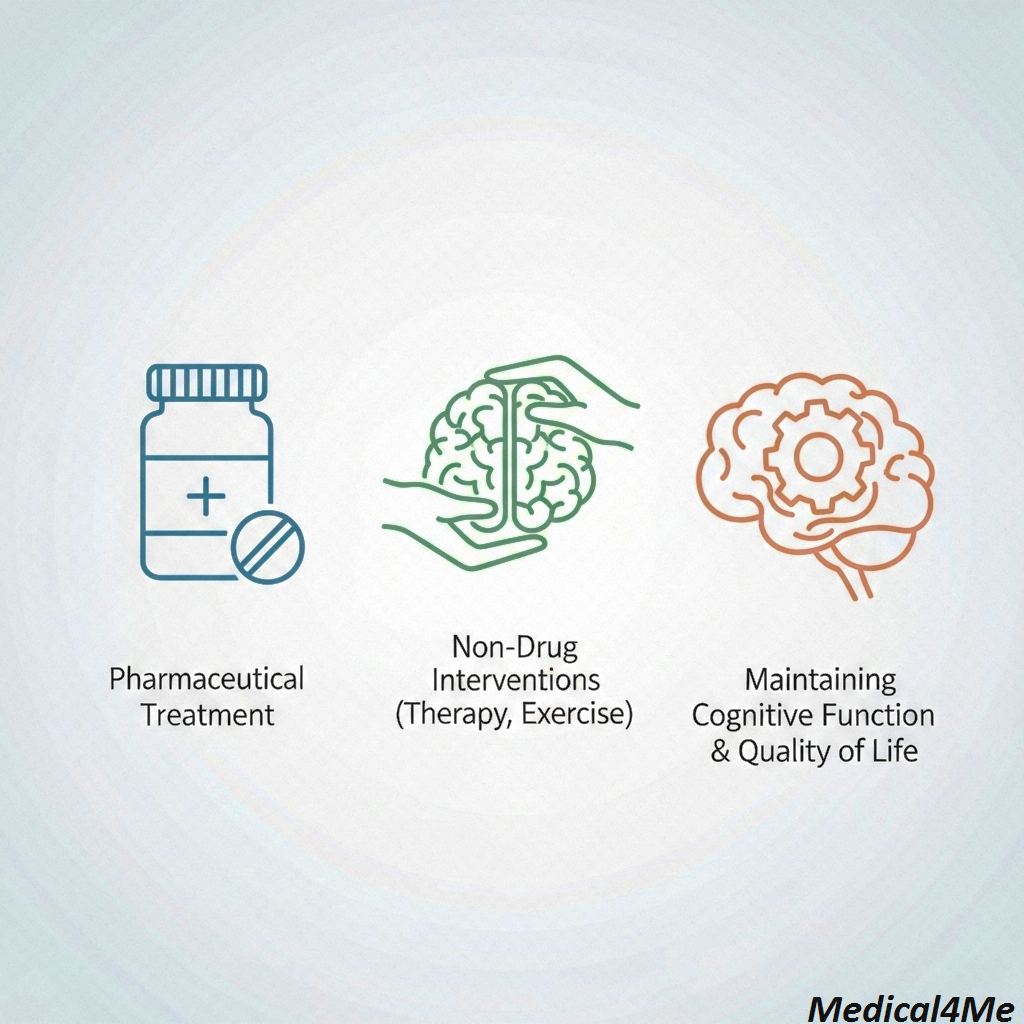
The introduction of the new antibody drugs like Lecanemab marks a significant shift. For the first time, we have a medicine that actually targets the amyloid plaques thought to cause the disease, rather than just managing the symptoms. But they’re not for everyone, and the risks must be carefully weighed by your physician. What I’ve learned is that the most successful management plans always combine appropriate drug therapy with robust non-drug interventions, maximizing overall brain health.
Prevention Strategies: Protecting Your Brain Health
Since a full cure for Dementia remains elusive, prevention and risk reduction are arguably the most powerful tools we have right now. The good news is that you have immense control over several modifiable risk factors. This is where true proactive health care begins.
The Pillars of Cognitive Prevention
- Move Your Body (Physical Activity): Regular exercise increases blood flow to the brain, which is crucial. Aim for 150 minutes of moderate-intensity aerobic exercise per week. Even brisk walking helps.
- Feed Your Brain (Diet): Adopt the MIND diet (a blend of the Mediterranean and DASH diets). It emphasizes leafy greens, berries, fish, and whole grains, and limits red meat and sweets. This directly supports better brain health.
- Keep Your Mind Engaged (Mental Stimulation): Continuous learning, reading, puzzles, or taking classes builds “cognitive reserve,” giving your brain more resilience against damage. Use it or lose it, basically.
- Stay Connected (Social Engagement): Social isolation is a major risk factor. Maintain an active social life; it keeps the brain stimulated and reduces risk. Join a club or volunteer.
- Manage Your Vitals (Cardiovascular Health): Aggressively control high blood pressure, diabetes, and cholesterol. As mentioned, vascular dementia is the second leading cause, and these conditions directly damage the brain’s blood supply.
And you know, even if you have a genetic risk, these prevention strategies can significantly delay the onset of symptoms. The key is consistency. It’s a lifelong commitment to brain health, not a temporary diet or exercise fad. The evidence is simply too strong to ignore.
When to Seek Medical Help: Distinguishing Forgetfulness from Dementia
Deciding when to talk to a medical professional about memory loss is difficult. It’s hard to bring up, and families often put it off. But an early cognitive assessment is crucial to rule out easily treatable causes and to start management of irreversible neurodegenerative conditions early. You should seek an immediate appointment if you notice certain severe signs.
⚠️ Urgent Indicators: When to Consult a Doctor Immediately
These signs suggest the need for an urgent diagnosis because they indicate a decline beyond normal aging:
- Difficulty Completing Familiar Tasks: Suddenly unable to drive to a nearby grocery store or manage the household finances.
- Chronic Disorientation: Repeatedly getting lost in places they know well, or being completely unsure of the current year or season.
- Personality Changes: Becoming unusually passive, fearful, or suspicious for no apparent cause, or having uncharacteristic aggression.
- Severe Judgment Errors: Making major financial mistakes or engaging in unsafe behaviors (e.g., leaving the stove on).
If the symptoms are sudden or rapidly worsening, that could indicate a stroke, severe infection, or adverse drug reaction—all of which require immediate medical attention. Don’t let fear delay getting the right health care.
A Patient Story: Hope Through Early Diagnosis and Management
I’ve seen patients who have spent months—even years—in denial. I recall Mr. Haroon, a retired engineer who came in because his daughter, Maria, was worried. He was always meticulous, but he started misplacing his wallet multiple times a day and couldn’t operate his bank’s mobile app anymore. Maria was heartbroken, convinced it was irreversible Dementia.
The initial cognitive assessment was concerning, but after a thorough diagnosis, including imaging, we confirmed a very early stage of Alzheimer’s. Mr. Haroon was devastated, of course, but he channeled that despair into action. We started him on an appropriate cholinesterase inhibitor medicine, and he became fiercely committed to brain health by joining a walking group and learning Spanish on his tablet. The treatment didn’t stop the disease, but it slowed the decline. He gained precious months of quality time, enjoying his grandkids and maintaining his independence, all because of that early diagnosis and proactive management. And you know, we always emphasize this kind of comprehensive care here at Medical4Me.
Latest Research & Developments: New Frontiers in Dementia Therapy
This is where the future of Dementia management lies. The research community is incredibly focused on finding treatments that stop the disease at its causes, not just its symptoms. And there is genuine hope on the horizon. Mayo Clinic explains the need for multiple therapeutic approaches.
1. Targeting Tau Tangles: While amyloid has dominated research, a shift is happening toward tau protein. Researchers at Johns Hopkins and the NIH are developing therapy targeting tau tangles, which seem to correlate better with the severity of cognitive decline than amyloid plaques. Clinical trials (Phase 2 and 3) are showing early promise in reducing tau spread, offering a potential second frontier in drug development.
2. The Blood-Brain Barrier Revolution (Focused Ultrasound): A truly cutting-edge treatment involves using focused ultrasound to temporarily open the blood-brain barrier. This allows drugs—including those new monoclonal antibodies—to penetrate the brain tissue far more effectively. According to recent trials, this could dramatically improve the efficacy of existing and future medicine that targets neurodegenerative conditions, fundamentally changing how we deliver therapy.
3. Artificial Intelligence for Early Diagnosis: AI is now being used to analyze retinal scans and speech patterns to detect subtle, pre-symptomatic signs of Dementia years before a clinical diagnosis can be made. This ultra-early diagnosis is vital because it would allow anti-amyloid and anti-tau drugs to be used when the damage to the brain is minimal, giving us the best chance at effective prevention.
Frequently Asked Questions My Patients Ask
Your Questions About Dementia Answered
No, Dementia is not a normal or inevitable part of aging. While mild forgetfulness can occur as we get older, true Dementia—a persistent and progressive decline in cognitive function that interferes with daily life—is caused by physical changes in the brain and requires a formal medical diagnosis and treatment plan. It’s a disease, not just getting old.
Absolutely. Lifestyle modifications are among the most effective prevention strategies. Managing heart health (blood pressure, cholesterol, diabetes) directly impacts brain health. Regular physical exercise, a heart-healthy diet, staying socially active, and continuous mental stimulation significantly reduce the long-term risk of developing some forms of Dementia.
The relationship is simple: Alzheimer’s is the most common cause of Dementia, but not the only one. Dementia is an umbrella term for a collection of symptoms related to severe cognitive decline. Alzheimer’s disease is a specific brain disease that causes these symptoms due to amyloid plaques and tau tangles. Other causes of Dementia include vascular issues and Lewy bodies.
Currently, there is no cure for most progressive forms of Dementia, like Alzheimer’s. However, certain medications (cholinesterase inhibitors and Memantine) can help manage and slow the progression of symptoms for a period. New monoclonal antibody therapies are also showing promise in targeting the underlying causes, giving real hope for future management.
The most critical support is patience, empathy, and structure. Establish a predictable daily routine to reduce confusion. Focus on maintaining dignity and connection, not testing their memory. Join a caregiver support group immediately. You need a support system for yourself so you can provide the best possible care for them.
The Path to Hope: Taking the Next Step in Dementia Care
We’ve walked through the emotional reality of Dementia, from recognizing the first subtle signs to the new frontiers of treatment. The key takeaway is simple: a diagnosis is not a period; it’s a comma. It marks the beginning of a new phase, one that demands proactive management, not surrender.
Here are your three most actionable next steps:
- Seek Clarity Early: If you or a loved one shows persistent symptoms of memory loss, request a full cognitive assessment immediately. Early diagnosis is your greatest asset.
- Prioritize Lifestyle: Commit to the pillars of prevention—physical activity, heart health care, and mental engagement. This improves overall brain health regardless of diagnosis.
- Build Your Team: Don’t try to manage this alone. Find a doctor specializing in neurodegenerative conditions and connect with caregiver support resources right away.
Remember Mr. Haroon. With early intervention and a dedicated approach, life after a Dementia diagnosis can still be rich, connected, and meaningful for many years. Don’t lose hope—take action today and start your journey with courage.

💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.