Understanding Diabetes Type 1: A Doctor’s Honest Guide
I know it’s late. Maybe you’re sitting there with a cup of tea that’s gone cold, scrolling through your phone because something feels off. Maybe you’ve noticed your child drinking water like they’ve just run a marathon, or perhaps you, yourself, have felt an exhaustion that sleep just won’t fix.
I’m Dr. Saqlain Mushtaq. Pull up a chair. Let’s talk about this not as doctor and patient, but as friends trying to make sense of a puzzle. I want to talk to you about Diabetes Type 1. It’s a term that carries a lot of weight, doesn’t it? But fear often comes from the unknown. So, let’s turn the lights on.
What Diabetes Type 1 Really Is
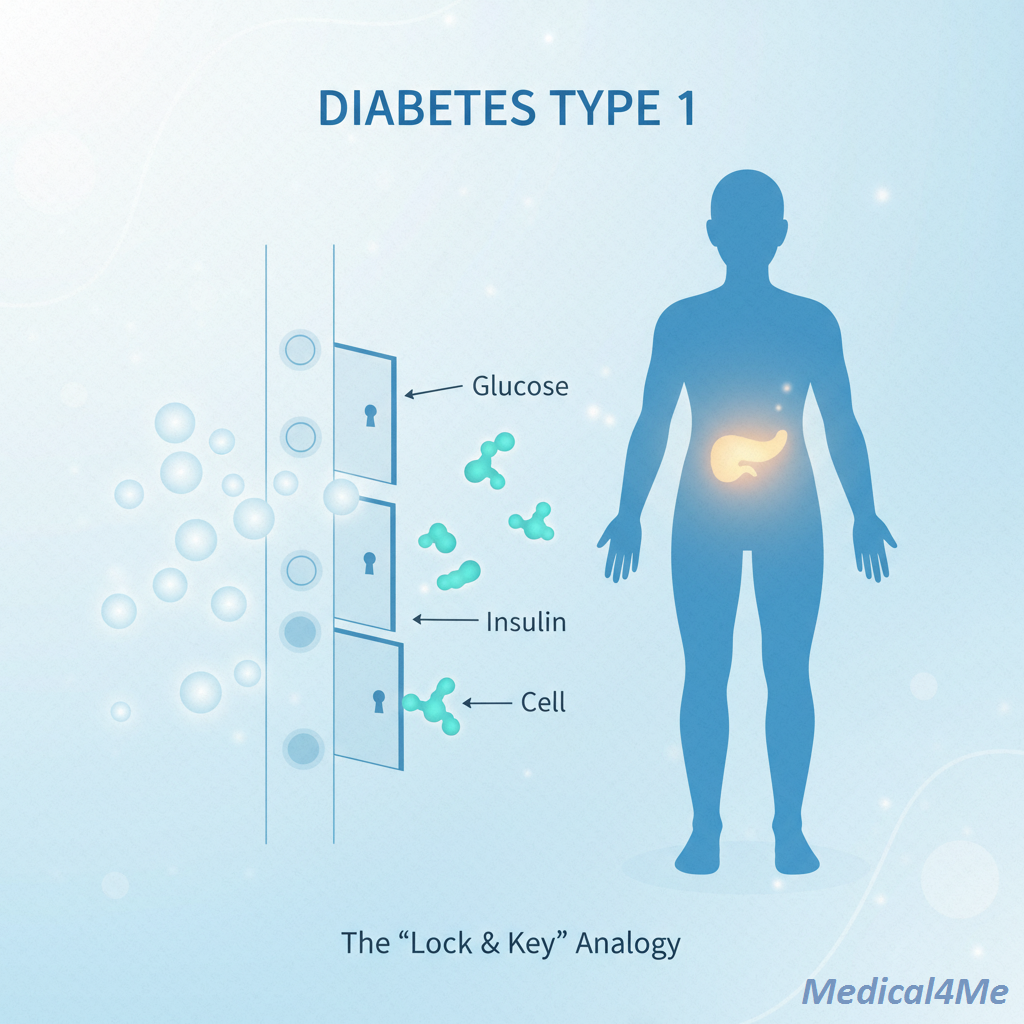
Imagine your body is a bustling city. For this city to run, it needs energy—specifically, glucose (sugar). Now, usually, there’s a key maker in town called the pancreas. It produces keys called “insulin” that unlock the doors to all the houses (cells) so the energy can get inside.
With Type 1 Diabetes, it’s like the key factory has suddenly gone on strike and shut down completely. The city is flooded with energy (sugar in your blood), but none of the houses can open their doors to let it in. The cells starve while surrounded by food.
My first thought when a patient describes this is always, “This isn’t their fault.” It’s an autoimmune reaction. Your body’s immune system, which usually fights off the flu or infections, got confused and attacked the key factory.
Take Haris, for example. He’s a 34-year-old graphic designer, When he first came to me, he wasn’t worried about sugar; he was worried about his vision. “Dr. Saqlain,” he said, “I can’t focus on my screens anymore.” He had lost 15 pounds in a month without trying. He thought it was just the stress of city life. It wasn’t. It was his body crying out for keys.
Recognizing the Symptoms
Because the cells are starving, your body starts shouting for help. However, these shouts can sometimes look like other things. Here is what you absolutely need to look for:
- Unquenchable Thirst: You drink a glass of water, and five minutes later, your mouth feels like the Sahara Desert.
- Frequent Urination: Because you’re drinking so much, and because your kidneys are trying to flush out the excess sugar, you’re in the bathroom constantly.
- Sudden Weight Loss: As I saw with Haris, you eat plenty, but the scale drops. Your body is burning fat and muscle for fuel because it can’t access the sugar.
- Extreme Hunger: You feel “hangry” all the time.
- Blurry Vision: High blood sugar pulls fluid from your lenses, affecting your focus.
- Fruity Breath Smell: This sounds strange, but it’s a sign of ketones (acid) building up.
Root Causes: The Honest Truth
To be perfectly honest, the medical community is still exploring the precise mechanism of why the immune system attacks the pancreas. We know genetics play a role, and we know environmental triggers (like a virus) might set it off. But we don’t have the full picture yet.
It’s frustrating, I know. But knowing what is happening is often more useful than knowing why when we are in the trenches of management.
The Diagnostic Journey
If you suspect this, don’t wait. The diagnosis process is straightforward. When I see a patient, here is the roadmap we follow:
- The A1C Test: This gives us an average of your blood sugar over the past 2-3 months. It tells me what’s been happening when you weren’t looking.
- Random Blood Sugar Test: We take a sample right then and there. If it’s 200 mg/dL or higher and you have symptoms, that’s a strong indicator.
- Fasting Blood Sugar Test: You don’t eat overnight, and we check you in the morning.
- Autoantibody Tests: This is the “smoking gun.” We look for the specific antibodies that are attacking the pancreas. This confirms it’s Type 1 and not Type 2, just like with other conditions where distinctions matter.
Treatment Reality
This is where people get scared. They hear “needles” and “forever.” But let me tell you about Zainab, a 52-year-old librarian. She was diagnosed late in life, which is rare but happens. She told me, “Dr. Mushtaq, I can’t live my life attached to a machine.” Today, Zainab hikes on weekends. She visits her family in every winter. She manages her condition; it doesn’t manage her.

Lifestyle Adjustments
You have to become a bit of a mathematician. You’ll learn to count carbohydrates. It’s not about never eating cake again; it’s about knowing that if you eat the cake, you need to provide the keys (insulin) to handle it.
Medical Options
Since the body can’t make insulin, we must replace it. There is no pill for this yet, sadly.
Common Medications (Insulins):
- Insulin Glargine (Lantus/Basaglar): This is your “background” insulin. It works slowly over 24 hours to keep things stable.
- Side Effects: Low blood sugar, weight gain, or injection site reactions.
- Insulin Lispro (Humalog): This is “mealtime” insulin. It acts fast (within 15-30 minutes) to handle the food you just ate.
- Side Effects: Ideally, it just lowers sugar, but if you take too much, it causes hypoglycemia (dangerously low sugar).
Here is how different delivery methods stack up:
| Feature | Insulin Injections (Pens) | Insulin Pump |
|---|---|---|
| Convenience | You carry a pen; simple but requires multiple shots a day. | Attached to your body; requires fewer sticks but you wear it 24/7. |
| Control | Good control, but less precise for tiny adjustments. | Excellent, precise control; mimics a real pancreas better. |
| Cost | Generally cheaper upfront. | Expensive hardware and supplies. |
| Visibility | discreet. | Visible device on your belt or arm. |
As I mentioned in recent posts, technology is moving fast. Continuous Glucose Monitors (CGMs) now send sugar readings to your phone every 5 minutes, so you don’t have to prick your finger constantly.
Red Flags: When to Call 911
We need to be serious for a moment. There is a condition called Diabetic Ketoacidosis (DKA). Remember the “fruity breath”? If the body runs out of insulin entirely, your blood turns acidic.
Look out for:
- Nausea and vomiting.
- Stomach pain.
- Confusion or difficulty staying awake.
- Deep, rapid breathing.
If you see this, don’t drive yourself. Call for help. CDC guidelines state that DKA is a medical emergency.
Frequently Asked Questions My Patients Ask
No. Unlike Type 2, Type 1 is autoimmune. Diet helps manage it, but it cannot cure it.
Absolutely not. Sugar intake does not cause Type 1 Diabetes. Please let go of that guilt.
Yes! In fact, exercise is great. You just need to monitor your levels, as Mayo Clinic explains in their activity guides.
Not necessarily. High sugar damages eyes over time. With good management, you can protect your vision.
Yes, but it requires planning. You’ll need tight control before and during pregnancy to keep the baby safe.
My Final Professional Advice
I want to leave you with one last story. Bilal, a 19-year-old college student. He plays cricket on the weekends and studies engineering. When he was diagnosed, he thought his life was over. He sat in my office, hoodie up, refusing to look at me.
I told him what I’m telling you: “You have a new job now. You are your own pancreas. It’s a part-time job you didn’t apply for, and the pay is zero, but the benefits are that you get to keep living your amazing life.”
Six months later, Bilal is thriving. He wears his insulin pump like a badge of honor.
If you have symptoms, go to the doctor. If you are diagnosed, take a deep breath. You are stronger than you think, and here at Medical4Me, we believe that with the right tools, you can handle anything.
As WHO data shows, millions live full, happy lives with this condition. You will too.


💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.