Fibromyalgia
I know it is late. I can almost picture you sitting there, rubbing your neck or your shoulders, wondering why you feel like you just ran a marathon when all you did was go to the grocery store. You have probably seen five different doctors. You might have been told, “It’s all in your head,” or “You just need to relax.”
I want you to listen to me very carefully: I believe you.
I am Dr. Saqlain Mushtaq, and tonight, we are going to stop the gaslighting. We are going to talk about Fibromyalgia—not as a mystery, but as a manageable reality.
Let me tell you about Mariam.
Mariam is a 32-year-old primary school teacher. She loves her job, but last year, she sat in my office in tears. She told me that when her students hugged her, it felt like burning sandpaper against her skin. She was exhausted, sleeping ten hours a night but waking up feeling like she hadn’t slept a wink. She thought she was losing her mind. She wasn’t. Her nervous system was just shouting when it should have been whispering.
We got Mariam back to the classroom. She isn’t “cured”—because this isn’t a cold—but she is happy, functioning, and smiling again. That is the goal for you, too.
What Fibromyalgia Really Is
To understand this condition, you have to stop looking at your muscles and start thinking about your brain.
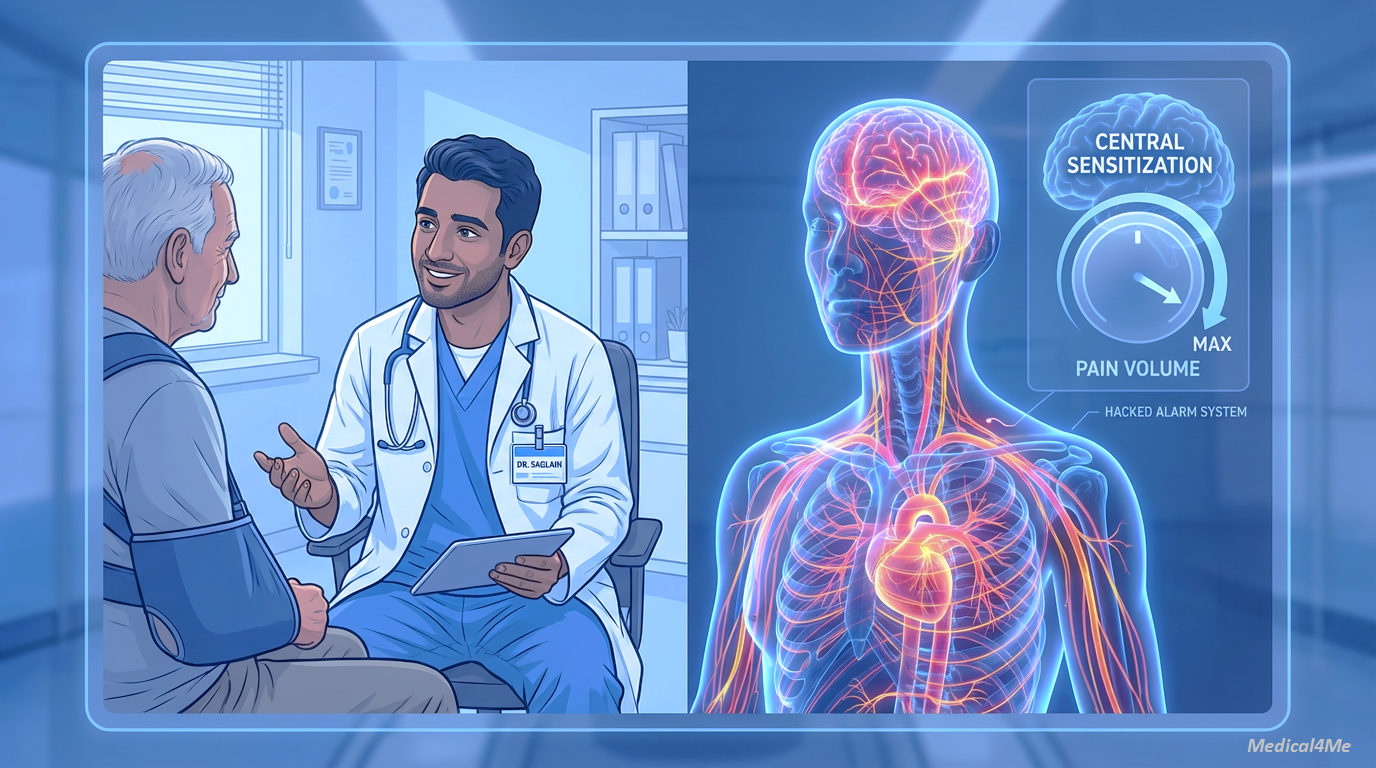
Imagine your body is a high-tech house protected by a security system. In a typical person’s house, the alarm only goes off if a burglar smashes a window. That is normal pain.
With Fibromyalgia, the security system has been hacked. The sensitivity dial has been turned up to the maximum level. Now, the alarm doesn’t just go off for burglars. It goes off when the wind blows. It screams when a cat walks across the lawn. It triggers when the mailman drops a letter.
Your body isn’t actually damaged—your muscles aren’t torn—but your brain is receiving a “DANGER” signal that is just as real as a broken bone. This is called “central sensitization.” It is a volume control problem, not a tissue problem.
My first thought when a patient describes this is always, “Okay, the hardware is fine, but the software is glitching. We need to reboot the system.”
Recognizing the Symptoms
Because this condition affects the central nervous system, it can feel like everything is going wrong at once. It is overwhelming.
However, there is a pattern to the chaos. Here are the specific signs I look for:
- Widespread Pain: This is a dull, aching pain that has lasted for at least three months. It has to be on both sides of your body and above and below your waist.
- The “Fibro Fog”: This is cognitive dysfunction. You walk into a room and forget why. You struggle to find the right word. It feels like your brain is wrapped in cotton wool.
- Non-Restorative Sleep: You might sleep for a long time, but you wake up tired. This is because your brain keeps interrupting the deep, restorative stages of sleep with bursts of awake-like brain activity.
- Sensitivity to Stimuli: Bright lights, loud noises, or strong smells (like perfume) might suddenly make you feel nauseous or anxious.
- Stiffness: Especially in the morning, you might feel like the Tin Man before he got his oil can.
Root Causes
This is the part where I have to be completely honest with you. To be perfectly honest, the medical community is still exploring the precise mechanism that triggers this initially. We don’t have one single “germ” or “gene” to blame.
However, we do see triggers.
Take Ali hassan, for instance. He is a 45-year-old software engineer, a brilliant guy. He never had pain issues until he was in a minor car accident. The injury healed in weeks, but the pain never stopped. For Ali Hassan, the physical trauma acted like a switch that flipped his nervous system into “fight or flight” mode, and it got stuck there.
Common factors include:
- Genetics: It often runs in families. If your mother has it, your risk is higher.
- Infections: Some illnesses appear to trigger or aggravate the condition.
- Physical or Emotional Trauma: This is huge. PTSD and Fibromyalgia are often cousins. The body keeps the score.
Because of this complex web of causes, we treat the whole person here at Medical4Me, not just the pain points.
The Diagnostic Journey
There is no blood test for this. There is no X-ray that lights up and says “Fibromyalgia.” This is why it takes so long to get an answer. It is baffling for patients.
Here is the process I use to get us to the truth:
- The History: We talk for a long time. I listen to how you describe your pain.
- The “Rule Out” Phase: We do blood work (CBC, thyroid, sedimentation rate) to make sure you don’t have Lupus, Rheumatoid Arthritis, or thyroid issues.
- The Widespread Pain Index (WPI): We map out exactly where you hurt.
- Symptom Severity Scale: We measure your fatigue and cognitive issues.
- The Diagnosis: If you have the pain pattern, the fatigue, and we have ruled out the other conditions, we can confidently say it is Fibromyalgia.
Treatment Reality
You cannot fix this with just a pill. You also cannot fix it with just yoga. You need a toolbox.
Lifestyle: The Foundation
I have a patient named Bushra, 62, a grandmother who loves knitting. When she stopped moving because of pain, she got worse. We started her on warm water therapy (exercising in a heated pool). The warmth soothed her sensors, and the movement kept her joints loose.
You must move. Low-impact exercise (walking, swimming, Tai Chi) is the single most effective treatment we have. It signals to your brain, “See? We moved, and we are safe.”
Medical Options
Sometimes, the volume is too loud for you to even think about exercise. That is where medication comes in. We use drugs to turn down the volume.
Common medications I prescribe include:
1. Duloxetine (Cymbalta):
This is an antidepressant, but we don’t use it for depression here. It increases serotonin and norepinephrine, chemicals that help control pain signals.
How it works: It boosts the body’s natural “pain dampening” system.
Side Effects: Nausea, dry mouth, or slight dizziness.
2. Pregabalin (Lyrica):
This was the first drug approved specifically for this. It targets the nerve cells directly.
How it works: It quiets the overactive neurons so they stop sending “DANGER” signals.
Side Effects: Weight gain, swelling in the hands/feet, and drowsiness.
3. Amitriptyline:
An older medication that is brilliant for sleep. We use tiny doses.
How it works: It helps you get into that deep, restorative sleep stage so your muscles can heal.
Side Effects: Morning grogginess and dry mouth.
Comparing Your Paths:
| Feature | Holistic Approach Only | Medication + Holistic |
|---|---|---|
| Immediate Relief | Low | Moderate |
| Long-Term Success | High (if consistent) | Very High |
| Side Effects | None | Possible (drowsiness, nausea) |
| Focus | Retraining the brain | Dampening the signal |
The Mayo Clinic explains that a combination approach usually yields the best results.
Danger Signs for you
While Fibromyalgia itself won’t damage your organs or shorten your life, you need to be alert for things that might be mimicking it.
Call Your Doctor if:
- You have redness, heat, or swelling in your joints (Fibro does not cause inflammation).
- You develop a rash, especially across your face (this could be Lupus).
- You have sudden weight loss or high fevers.
Frequently Asked Questions My Patients Ask
No. The pain is 100% real. It is produced by the brain, but that doesn’t make it imaginary. It makes it neurological.
Not officially. However, many of my patients feel better when they reduce sugar and processed foods, which can be inflammatory.
No. Fibromyalgia causes pain and fatigue, but it does not damage the muscles or joints. It is not a degenerative disease.
It varies. Some women actually feel better during pregnancy due to hormonal shifts, while others struggle with the added physical stress.
Yes. Most people continue to work. We might need to adjust your schedule or ergonomics, but disability is not inevitable.
My Final Professional Advice
I want to go back to Mariam, the teacher.
She still has bad days. When the weather changes drastically, or when stress is high, her “security system” beeps. But she knows what it is now. She doesn’t panic. She takes a warm bath, she takes her meds, and she rests without guilt.
You have to stop fighting your body. Stop being angry at it for hurting. It is trying to protect you, even if it is doing a bad job of it right now.
As I mentioned in recent posts, recovery isn’t a straight line. But you can get your life back. You can lift your grandkids. You can go for that walk.
Be patient with yourself. You are resilient. And remember, this diagnosis is the beginning of the solution, not the end of the world.
Now, try to relax your jaw (I know you are clenching it). Get some rest. We will tackle this.


💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.