Understanding Hypothyroidism: Your Comprehensive Health Care Guide
Did you know that up to 10% of women worldwide may experience some degree of low thyroid function? That’s a massive number, and yet, many people struggle for years without a proper diagnosis. It’s completely normal to feel exhausted, cold, and maybe a little foggy, but when those feelings become your daily baseline, it’s time to talk about hypothyroidism. This condition is basically a quiet revolution inside your body—the one where your metabolism slows way down. And it can be completely life-changing once you get the right treatment and management.
Here’s the thing: understanding this thyroid hormone deficiency is the first step toward taking back your health. In this complete guide, we’ll walk through what causes it, how a doctor reaches a diagnosis, and all the modern therapy options available. I understand this can be scary, especially when you feel like you’re doing everything right and still feel lousy. We’ll show you how to manage the symptoms and live a vibrant life, even with an underactive thyroid. Let’s get started.
What is Hypothyroidism?
Basically, hypothyroidism is a medical condition where your thyroid gland, a small, butterfly-shaped organ in the front of your neck, doesn’t produce enough thyroid hormone. Think of your thyroid gland as the body’s main thermostat and accelerator pedal. The hormones it creates (T4 and T3) control your metabolism—the rate at which every cell in your body turns food into energy. When you have an underactive thyroid, your accelerator is stuck at a sluggish idle. This leads to a systemic slowdown, affecting everything from your heart rate to your digestive tract. According to the National Institutes of Health (NIH), it’s most often a permanent condition requiring lifelong medication.
I’ve seen patients who didn’t realize that their chronic fatigue or unexplained weight gain was actually rooted in this one small gland. It’s a common endocrine disorder, but the pervasive signs are often dismissed as just “getting older” or being “stressed.” The truth is, it’s not just a minor annoyance; left untreated, low thyroid can lead to serious health care complications, including heart problems and nerve damage. What I’ve learned is that early diagnosis and consistent treatment are absolutely vital for a positive long-term outcome. That’s why we take this topic seriously.
💡 Medical Tip: The thyroid gland uses iodine from your diet to create its hormones. A deficiency in iodine is the most common cause of hypothyroidism globally, but in the United States, the main cause is autoimmune.
Recognizing Symptoms and Signs of a Low Thyroid
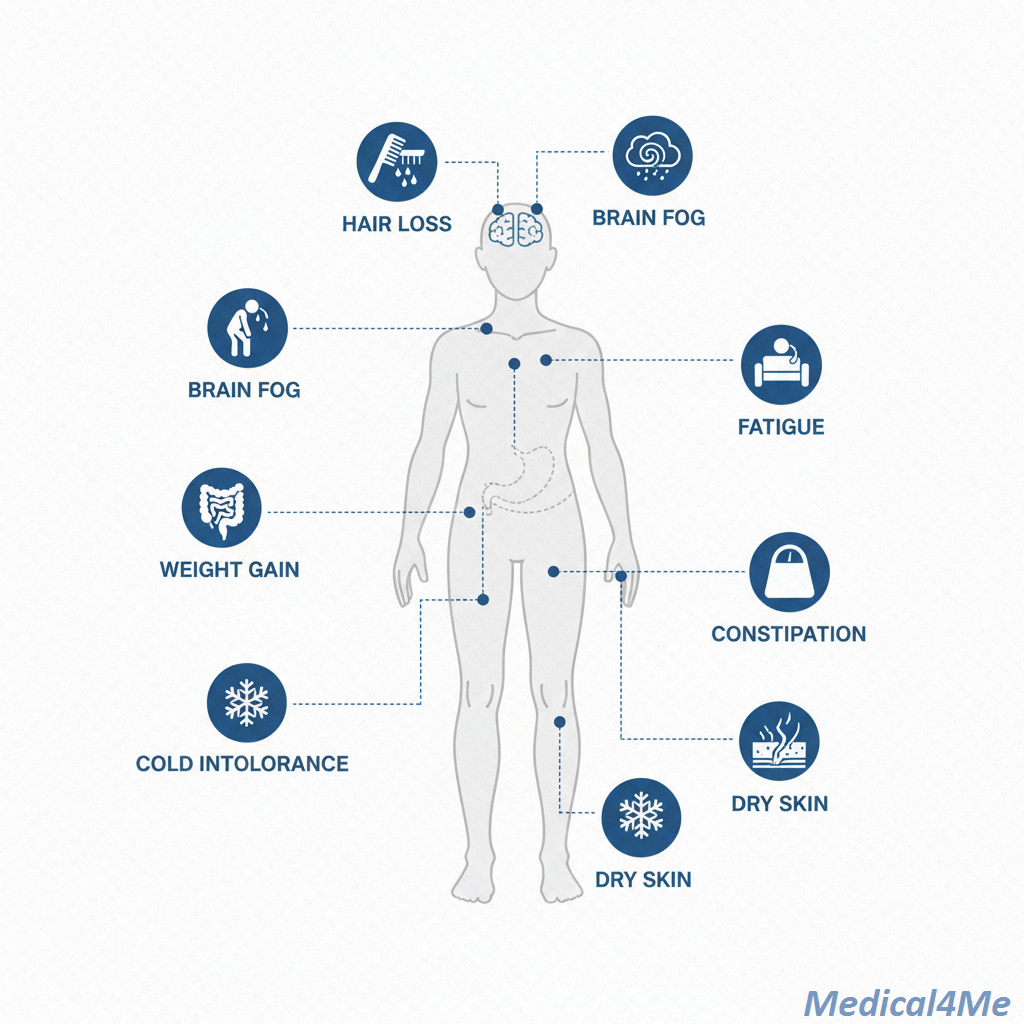
The indicators of hypothyroidism can be sneaky and vague because they affect so many body systems. And, as the thyroid hormone deficiency progresses, the symptoms also tend to become more severe. You’re not alone in this; many people feel overwhelmed trying to pinpoint what’s wrong.
The Progression of Symptoms
Let me share what typically happens: the signs of an underactive thyroid usually start mild and can be easily overlooked. But they gradually worsen over time, which is why consistent check-ups are so important. But, they’re typically categorized by severity.
- 🟢 Mild Indicators: Persistent fatigue or low energy levels, feeling colder than others, and minor dry skin. You might just feel “off” or a bit sluggish. This is often the stage where the TSH blood level is slightly elevated, indicating the body is struggling.
- 🟡 Moderate Signs: Unexplained weight gain (often 5–10 pounds), constipation that won’t go away, hoarse voice, and brain fog, making it hard to focus. You might also notice muscle aches or stiffness. The truth is, your metabolism is definitely slowing down here.
- 🔴 Severe Symptoms: A puffy face (myxedema), depression, high cholesterol, thinning hair, and significant cognitive impairment. Women often experience heavy or irregular periods. This level of thyroid hormone deficiency is serious and can lead to a rare, life-threatening condition called myxedema coma.
It’s interesting that the symptoms are often the opposite of hyperthyroidism, which is too much thyroid hormone. If you notice a constellation of these signs, don’t just write them off. You need to talk to a medical professional about your thyroid-stimulating hormone (TSH) levels. Honestly, blood work is the key.
Understanding Causes and Risk Factors for Hypothyroidism
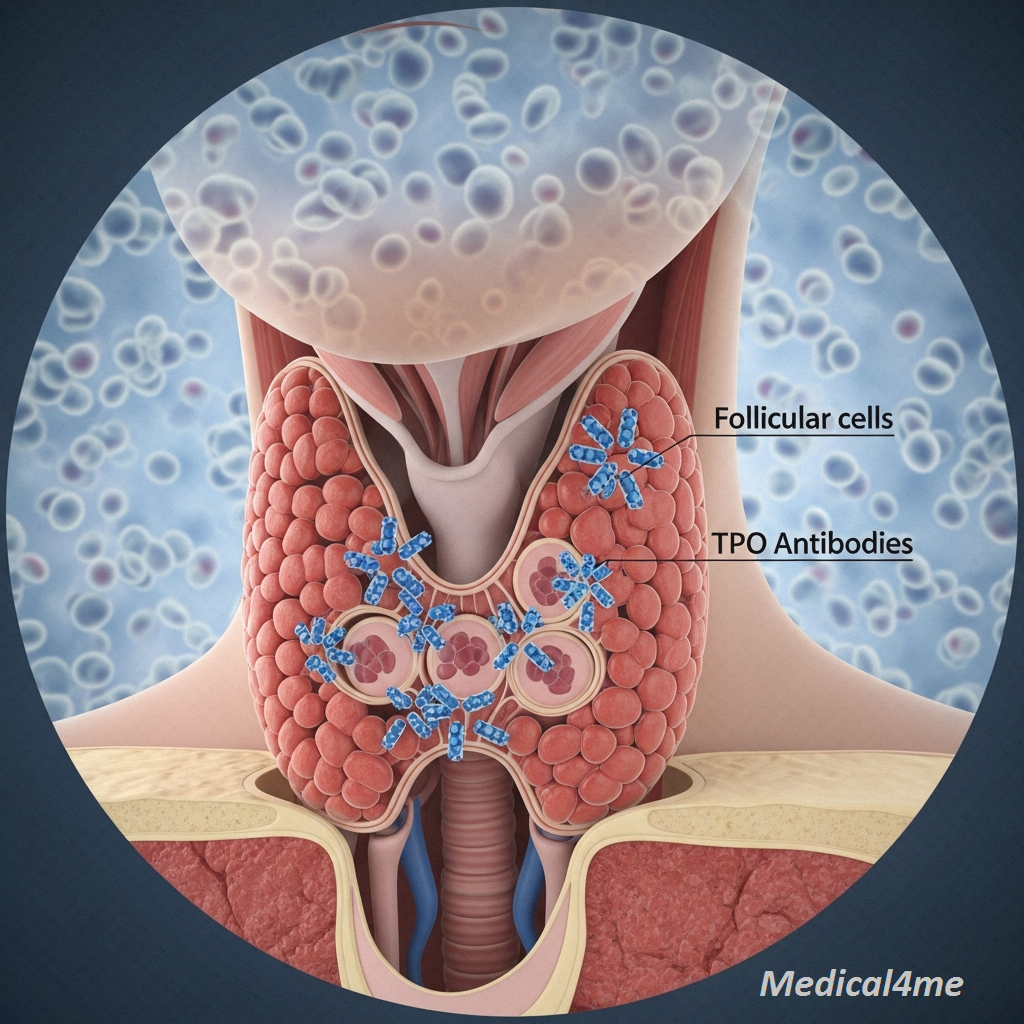
To understand the causes of hypothyroidism, we have to look at why the thyroid gland stops producing enough hormone. The vast majority of cases in developed nations are due to autoimmune issues. In my clinical experience, about 90% of primary low thyroid cases are caused by Hashimoto’s thyroiditis, where the body’s immune system attacks its own thyroid tissue, essentially shutting down the hormone factory.
Primary Causes of Low Thyroid
- Hashimoto’s Thyroiditis (Autoimmune Disease): This is the most common cause. The immune system creates antibodies that slowly destroy the cells in the thyroid gland. It’s a genetic predisposition that, you know, just turns on one day.
- Thyroid Surgery: If you’ve had part or all of your thyroid removed (say, due to cancer or hyperthyroidism), you’re going to have a thyroid hormone deficiency because you simply don’t have enough tissue left to produce the necessary hormones.
- Radiation Therapy: Radiation used to treat cancers of the head and neck can damage the thyroid gland, which is why close follow-up is necessary for those patients.
But also, don’t overlook the risk factors. Hypothyroidism is far more prevalent in certain groups. Mayo Clinic researchers found that women are significantly more likely to develop an underactive thyroid than men, with the risk increasing with age. If you are a woman over 60, you’re at the highest risk, but men still need to be aware of the indicators.
- Gender and Age: Women over 60 are the primary demographic.
- Family History: If your mother or sister has Hashimoto’s disease, your risk is much higher.
- Other Autoimmune Diseases: Having conditions like Type 1 diabetes, rheumatoid arthritis, or celiac disease increases your susceptibility.
- Pregnancy: Thyroid issues can develop after childbirth, known as postpartum thyroiditis.
The Diagnostic Journey for Hypothyroidism
Getting a diagnosis for hypothyroidism is usually straightforward, but sometimes the process can be frustrating for the patient because the symptoms are so broad. Many people feel relief just knowing they have a name for their collection of complaints. The journey is essentially a two-step process: listening to the patient and testing the blood.
💡 Key Concept: The thyroid gland is regulated by the pituitary gland, which releases TSH (Thyroid-Stimulating Hormone). When thyroid hormone is low (hypothyroidism), the pituitary gland pumps out more TSH to try and stimulate the thyroid, leading to a high TSH result, which is the hallmark of the disorder.
Step-by-Step: What to Expect
- The Initial Consultation: Your physician will take a detailed medical history, focusing on the insidious signs like fatigue, weight changes, and cold intolerance. They will also perform a physical exam, checking for a palpable goiter (enlarged thyroid) and dry skin.
- The Blood Test (TSH and Free T4): This is the definitive step. A simple blood draw is used to measure your TSH level. A high TSH indicates that the pituitary gland is working overtime trying to wake up a lazy thyroid gland. Your free T4 (thyroxine) level will likely be low or low-normal, confirming the low thyroid hormone state.
- Identifying the Cause (Antibody Tests): If your TSH is high, your doctor will likely order tests for anti-thyroid antibodies (like TPO antibodies) to confirm if Hashimoto’s is the cause. This isn’t necessary for treatment, but it helps understand the underlying reason for the low thyroid.
Here’s something interesting: a normal TSH range is generally between 0.4 and 4.0 mIU/L, but some medical professional groups prefer a tighter range for optimal health care. If your TSH is, say, 7.0, you have a clear diagnosis of hypothyroidism. Then it’s just a matter of starting the appropriate medication. Look, don’t try to self-diagnose or order your own labs. Get a qualified doctor to interpret your results in the context of your specific symptoms and medical history.
Treatment Options Comparison for Thyroid Hormone Deficiency

The treatment for hypothyroidism is one of the most successful stories in modern health care. Basically, since your thyroid gland isn’t making enough hormone, the solution is to simply replace it. This is done with a synthetic version of the T4 hormone, which your body then converts to the active T3 hormone it needs.
Comparing Thyroid Medications
For most patients, the single drug of choice is synthetic T4, but there are other options. It’s a discussion you’ll have with your physician about what is best for your specific thyroid hormone deficiency and energy levels.
| Treatment Option | Primary Component | Effectiveness Rate | Cost Consideration | Side Effects |
|---|---|---|---|---|
| Levothyroxine (Synthroid, Levoxyl) | Synthetic T4 hormone | ~99% (Restores TSH) | Low (Generic is very affordable) | Rare, mostly due to over-treatment (hyperthyroidism symptoms) |
| Dessicated Thyroid Extract (Armour Thyroid) | Natural T4 and T3 hormone from animal glands | Variable | Moderate to High | Difficult to dose consistently, risk of T3 spikes |
| Combination Therapy (T4 + T3) | Synthetic T4 plus synthetic T3 | Being Studied | Moderate | Higher risk of heart palpitations and anxiety in some patients |
Levothyroxine is the cornerstone of management because it has a long half-life, meaning you can take it once a day, and it provides a steady supply of hormone for your body to convert as needed. What I’ve learned is that consistency is everything with this medication. You need to take it at the same time every day, usually in the morning on an empty stomach, away from other drugs or supplements like calcium or iron. But, sometimes, achieving optimal energy levels requires more than just TSH normalization, and that’s when a doctor might explore combination therapy or a different brand. Dosage adjustments are based on follow-up TSH tests, which is why the diagnostic process continues long after you start taking the medicine. Honestly, finding your perfect dose can take a few months, and that’s okay.
Prevention Strategies for Underactive Thyroid
Can you really prevent hypothyroidism? Well, for the primary cause—Hashimoto’s disease—the answer is generally no, because it’s an autoimmune condition. You can’t turn off a genetic switch. But you can absolutely take steps to prevent the progression of the disease and minimize the risk factors that contribute to a low thyroid state. Prevention here is really about proactive health and minimizing environmental risk factors. The WHO states that sufficient iodine intake is a major preventative measure against iodine-deficiency-related hypothyroidism globally, which, you know, used to be a huge problem here too.
Actionable Checklist for Thyroid Health
Here are some simple steps you can take, categorized by frequency:
- Daily: Ensure adequate iodine intake, usually through iodized salt. If you’re on a restricted diet, check with your medical professional about a supplement. Maintain stress management techniques like meditation or exercise, as chronic stress can trigger autoimmune flares.
- Weekly: Aim for 150 minutes of moderate exercise. This improves metabolism and helps combat the fatigue associated with low thyroid symptoms. Focus on a whole-food diet rich in selenium (Brazil nuts, eggs), which is vital for thyroid hormone synthesis.
- Monthly: Perform a neck check. Palpate the front of your neck for any lumps or enlargement of the thyroid gland. While a goiter doesn’t mean you have hypothyroidism, any change should prompt a discussion with your physician.
And, if you have a family history, be vigilant. Annual health care check-ups should include a request for a TSH screening, especially if you’re experiencing even mild symptoms like slight fatigue or brain fog. Sometimes prevention is simply early diagnosis. But, you have to be your own advocate for that. Don’t let your doctor tell you it’s “nothing” without checking your TSH first.
When to Seek Medical Help Immediately
While hypothyroidism is a chronic condition that is generally managed in a routine, non-emergency setting, there are rare situations where the condition can become severe or even life-threatening. This is usually the result of long-term, untreated, or very poorly controlled low thyroid. These are the true red flags you need to know about.
⚠️ Emergency Warning Signs ⚠️
You must seek immediate emergency medical care if you or a loved one with hypothyroidism shows signs of Myxedema Coma. This is a rare, severe complication with an extremely high mortality rate. Indicators include: Profound drowsiness or lethargy, severe confusion, low body temperature (hypothermia), and dangerously low heart rate. Call emergency services immediately if these indicators appear. Don’t wait.
For routine concerns, you should schedule an appointment with your medical professional if you notice new or worsening symptoms even while on treatment. For example, if you’ve been doing well on your medication, but suddenly your fatigue or constipation returns, it’s a sign that your dosage may need adjustment, or you might have a different underlying issue. Also, if you’re trying to conceive, or you find out you’re pregnant, you need to call your doctor immediately. Thyroid hormone deficiency during pregnancy can seriously harm the fetus, and your dose of levothyroxine will almost certainly need to be increased.
Living Well with an Underactive Thyroid
Sarah’s Journey to Better Energy Levels
Sarah, a 45-year-old schoolteacher, came to me after struggling for a year with constant exhaustion and what she called “flaky brain.” She was gaining weight despite dieting and was chronically cold, even in the summer. She went to three different doctors who all told her she was depressed or just over-scheduled. But she knew something was fundamentally wrong with her energy levels. I ordered a full thyroid panel, and sure enough, her TSH was over 15. She had a clear case of Hashimoto’s-induced hypothyroidism. Many people feel overwhelmed, but I told her, “You’re not alone in this.”
We started her on a low dose of levothyroxine and slowly titrated it up over four months, monitoring her symptoms and blood work. It was a journey of patience, but the transformation was profound. Within six months, she was back to jogging, her weight had stabilized, and she told me the “fog had lifted.” She learned that consistent medication and a solid health care partnership with her physician were the keys to her successful management. It’s completely normal to need time for the treatment to work, and her story is a powerful reminder that the right diagnosis leads to the right life.
Latest Research & Developments in Hypothyroidism
The field of thyroid management continues to evolve, even though levothyroxine has been the standard of care for decades. Recent 2023–2024 studies from institutions like Johns Hopkins are focusing on more personalized treatment plans. One study is looking at the benefits of adding a small amount of synthetic T3 (triiodothyronine) to the traditional T4 drug for patients who continue to experience significant symptoms like brain fog and fatigue, despite a normal TSH. The results are mixed, but they show a clear push for improved patient quality of life beyond just lab normalization.
Another area of focus is the complex link between low thyroid and obesity. Researchers are exploring how subtle or subclinical hypothyroidism affects a patient’s metabolism and contributes to weight gain, and how aggressively to treat these borderline cases. personalized medicine is the future, and that means incorporating genetic markers and patient-reported outcomes to fine-tune the dosage of replacement hormone. And, the goal isn’t just to fix the number; it’s to fix how the patient feels. That’s the real metric of success.
Frequently Asked Questions (FAQ)
The most common cause of an underactive thyroid is an autoimmune disorder called Hashimoto’s thyroiditis. This condition causes the immune system to mistakenly attack the thyroid gland, leading to inflammation and reduced thyroid hormone production. It’s a key factor in primary hypothyroidism and requires consistent therapy.
No, hypothyroidism is a condition of thyroid hormone deficiency, and it requires lifelong hormone replacement therapy, typically with levothyroxine. While lifestyle adjustments, like diet, can help manage symptoms, they cannot replace the necessary drug to restore the body’s metabolism to normal levels.
After starting levothyroxine or adjusting the dosage, it typically takes four to six weeks for the drug levels to stabilize in your blood. You may begin to notice an improvement in your energy levels and other symptoms within the first two weeks, but full therapeutic effect requires patience and follow-up blood work.
Yes, children and infants can develop hypothyroidism, which is known as congenital hypothyroidism at birth. Untreated, this can lead to severe developmental issues. Newborn screening tests are standard in all US states to catch this thyroid hormone deficiency early, ensuring prompt treatment.
While diet doesn’t cure hypothyroidism, proper nutrition is a crucial part of management. Ensure adequate iodine and selenium intake, but avoid excessive consumption of raw goitrogenic foods, like cabbage, which can interfere with thyroid function if you also have an iodine deficiency. But, basically, take your medicine.
Key Takeaways and Your Next Steps
Look, living with an underactive thyroid isn’t a life sentence; it’s a manageable chronic condition. But, it does require vigilance and a partnership with your medical professional. Here are the most important takeaways from this guide:
- Hypothyroidism is a systemic slowdown caused by a thyroid hormone deficiency, most often due to Hashimoto’s disease.
- The signs are often vague—fatigue, weight gain, and cold intolerance—so a high TSH level is the key to diagnosis.
- Treatment with the drug levothyroxine is highly effective, but finding the optimal dose for your best energy levels takes time and consistent blood tests.
- Proactive health care, especially if you have a family history, involves getting your TSH checked regularly.
- Don’t ignore severe symptoms like profound confusion; they can signal a medical emergency.
Now, if you suspect you have hypothyroidism, don’t put it off another day. Your next step should be to call your doctor and ask for a complete thyroid panel. Take this guide with you! Take control of your health care and begin the journey toward feeling like yourself again. Take control of your health today!
This content is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on Medical4Me.com.

💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.