What Hives Really Are
In the more esoteric medical terms, we call them urticaria. That word doesn’t make them itch any less. Hives are those items that suddenly appear to be raised, red, or skin-colored variants, such as welts.
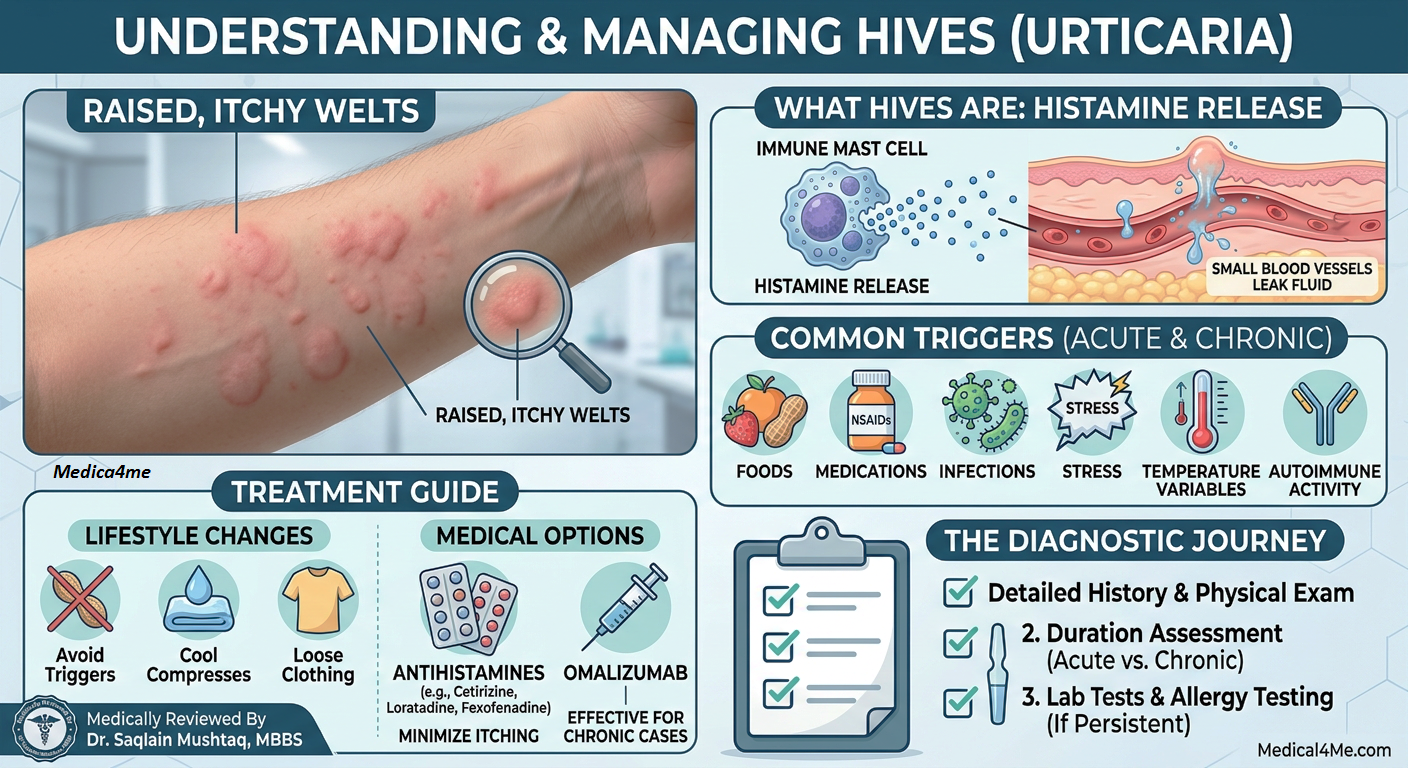
The immune system secretes histamine, which causes small blood vessels to leak fluid and cause swelling. What would happen if the security guard at your house turns the fire alarm on for burnt toast? The reaction is real, even when the threat just isn’t dangerous.
According to Mayo Clinic, acute hives usually are common and resolve themselves in weeks. WHO data illustrates that allergic conditions like this affect millions of people all over the world.
Recognizing the Symptoms
Safiya, a 34-year-old software engineer, came to me terrified during a sudden outbreak before a presentation. Her symptoms were these which is following below:
- Red or skin-colored welts which are raised
- Intense itching
- Change in shape and location of lesions (moving spots)
- Slight swelling around lips or eyelids
- Rash worsening with heat
Typically, individual spots disappear within 24 hours even if new ones appear in other places. The first thing that comes to mind when one is describing a condition of moving, itchy welts is histamine-driven urticaria.
Some Causes of Hives
Farhan, 52, a teacher of literature, had trouble with hives for six weeks. We searched for triggers. Sometimes we find them, and sometimes we do not. Medicine still has not figured out why chronic spontaneous hives occur without having a clear cause.
Common triggering factors include:
- Foods
- Medications (NSAIDs, for example)
- Infections
- Stress
- Temperature variables
- Autoimmune activity
With conditions like this, as with any other illness, just because you can’t find a cause doesn’t mean there’s any danger.
The Diagnostic Journey
Most cases of acute hives are not worth doing much testing on unless there are some really nasty symptoms. However, if we do investigate, the process looks like this:
- Detailed history including timing and triggers
- Physical examination
- Looking at duration (acute vs. chronic)
- Basic lab tests should it persist
- Allergy testing if necessary

Treatment:
Lifestyle must be Change:
Affected skin is best treated by avoiding known triggers, using loose clothing, keeping the skin cool, and avoiding stress. Cold compresses may bring itchiness under control soon.
Medical Options
Common antihistamines include Cetirizine, Loratadine, and Fexofenadine. They block the histamine receptors and minimize itchiness. Side effects may include mild drowsiness, headache, or a dry mouth.
Resistant cases may require the use of injections of Omalizumab under supervision.
| Treatment Option | Pros | Cons |
|---|---|---|
| Antihistamines | Quick relief, safe over the long term | May cause drowsiness |
| Omalizumab | Effective for Chronic cases | Expensive, injections required |
Clinical Indicators of Serious Pathology
While usually harmless, you should go to Urgent Care when you see:
- Swelling of tongue or throat
- Difficulty breathing
- Chest tightness
- Fainting
Frequently Asked Questions
Are Hives contagious?
No. There is no one to catch them from.
Can stress really cause them?
Yes. Stress is a way of shifting the balance of immunity and can result in outbreaks.
Can Hives become permanent?
Chronic hives can be present for months or years, but the majority of them disappear.
💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.