Anxiety Disorders: symptoms, causes, diagnosis, and care
Anxiety happens a lot. Many people are surprised to discover that it often manifests itself as physical signs of stress – a racing heart, a tight chest or upset stomach – before they think about it as being a mental health problem. According to recent surveys that have been conducted by the CDC, approximately one-third of adults have experienced symptoms of anxiety over the past few weeks. This means anxiety is not unusual in the everyday health care setting.
Anxiety does not necessarily seem dramatic. It can manifest itself in silent avoidance and restless sleep. When worry, fear or panic persists for a long enough time and it starts to interfere with everyday life we call this an anxiety disorder. In my clinical experience providing a good explanation can alone help diminish fear. Clear information helps.
This Post describes what anxiety disorders are, how they manifest their symptoms and signs, the known causes and risk factors, the appearance of a diagnosis visit, and how the treatment options compare with each other. It includes prevention strategies and safety signs as well.
What are Anxiety disorders?
Anxiety happens a lot. Many people are surprised to discover that it often manifests itself as physical signs of stress – a racing heart, a tight chest or upset stomach – before they think about it as being a mental health problem.
These diagnoses include generalized anxiety disorder (GAD), panic disorder, social anxiety disorder, specific phobias, and other anxiety-related disorders.
According to recent surveys that have been conducted by the CDC, approximately one-third of adults have experienced symptoms of anxiety over the past few weeks. This means anxiety is not unusual in the everyday health care setting
This Post describes what anxiety disorders are, how they manifest their symptoms and signs, the known causes and risk factors, the appearance of a diagnosis visit, and how the treatment options compare with each other. It includes prevention strategies and safety signs as well.
However, the feeling of anxiety is not a single one. It may occur in the form of looping concerns, flashpoints of fear and that frozen fear which appears like a burden in your body. And how long it sticks around, how hard it hits, how it changes the way you act – especially avoiding stuff, and needing reassurance – doesn’t matter if it’s all just ‘more stress.’ Stress usually has a definite trigger and it disappears.
Anxiety can grab on to any number of triggers, change all the time, and never stop when things are ok in your life. It is the obstinacy that AA-typically causes folks to visit the doctor.
Symptom and signs identification:
What a person experiences is called the symptoms. Signs are what other people are able to see. An indicator can be either. This is useful, since anxiety may be felt internally but on the outside may be “normal.”
NIH notes the prevalence of panic disorder is lower than that of generalized anxiety symptoms (2 – 3% of adults a year).
- 🟢 Mild indicators: restlessness, irritability, faint has trouble sleeping, stiff muscles and worry that you can still most days change.
- 🟡 Moderate indicators: Thinking too much, trouble being able to concentrate much, avoiding things, upset stomach and headaches, sweating or trembling.
- 🔴 Severe indicators: Panic Attacks, Strong Avoidance Limit Work or Relationships, Constant Sleeplessness, Intense Bodily Symptoms Feel Like a Medical Emergency – Am I Being Erased by a Stroke?Severe Indicators: Panic Attacks Strong Avoidance Limit Work or Relationships Constant Sleeplessness Intense Bodily Symptoms Feels Like a Medical Emergency Reported Indicators of a Stroke – Is What I’m Experiencing a Stroke?
The timeline differs. Some people are slow builders of worry and tension. Others have episodes of sudden panic that evoke the avoidance of risky situations, such as driving or being around crowds. That evasion may soon narrow down life.
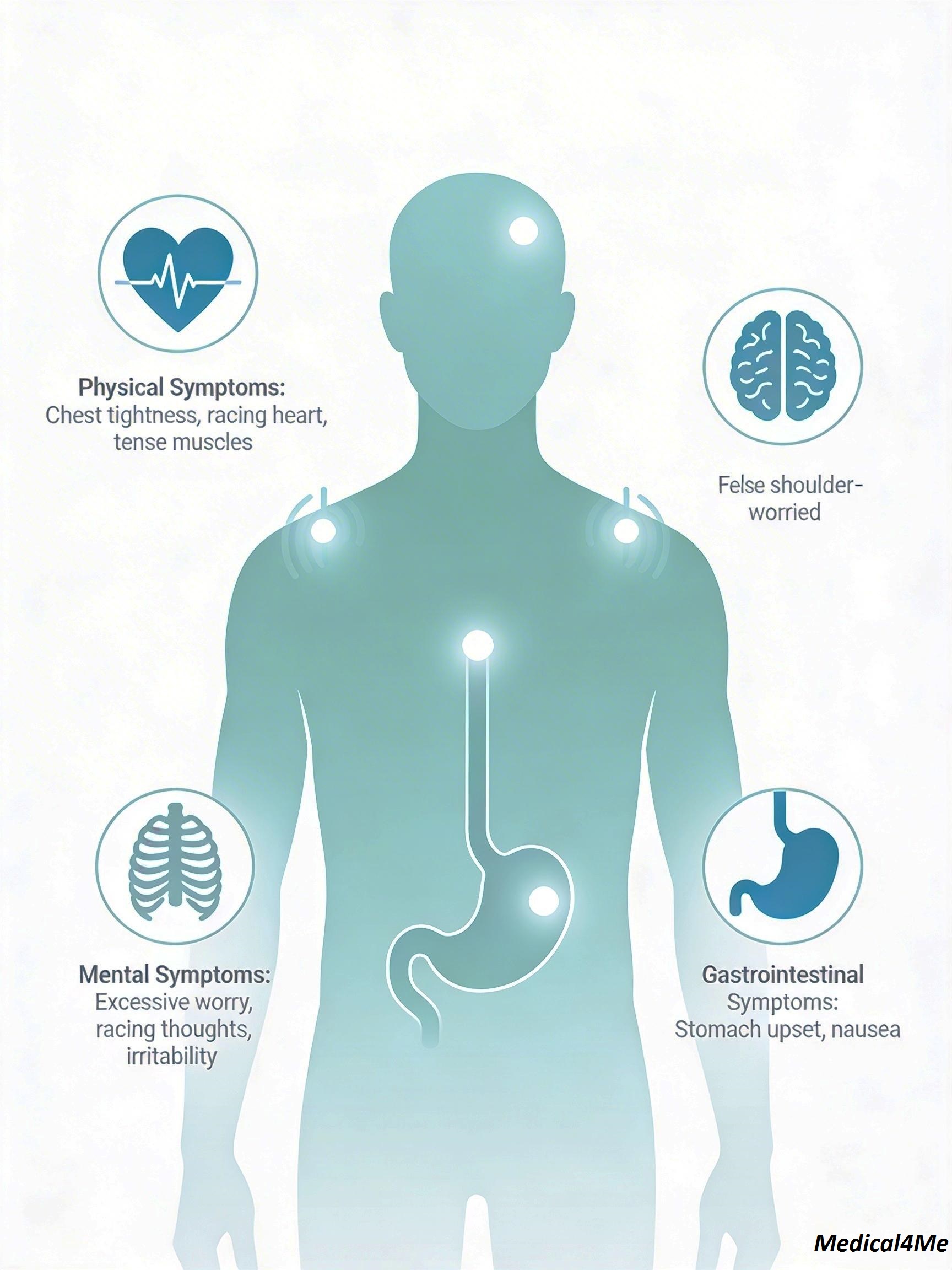
Symptoms can overlap with other health conditions. New or severe physical symptoms deserve medical evaluation.
So, what tends to push symptoms from manageable to unmanageable? Often it’s the combination of poor sleep, ongoing stress, and repeated avoidance. Honestly, that trio is a common story in clinic. Common, and very treatable.
Related reading on Medical4Me: panic attack symptoms.
Understanding causes and risk factors
It almost happens never because of a single cause. It has more to do with accumulated risk factors. Some are biological, some are learned, some are medical and some are social or environmental.
Genetic Research has shown the role of genetics. About 30 – 40% of the risk is due to genes.
- Family history: When one of your close relatives has anxiety illness, there is a higher risk that you also will but not sure.
- Temperament and learning: Uncertainty is riskier! That is what the brain can learn about basically due to high sensitivity and early experiences. Therapy can help to undo that lesson.
- Chronic stress load: Ongoing stress such as caregiving, financial issues or job stress keep the stress system on.
- Medical contributors: Physical health problems including thyroid problems, anemia, heart rhythm problems, asthma, balance problems, or chronic pain, may also increase anxiety or mimic the symptoms.
- Substances and medicines: Too much caffeine, nicotine, stimulants, alcohol withdrawal or some prescription medications can make anxiety much worse.
When anxiety comes on abruptly, doctors often turn to caffeine, sleep, alcohol and recent medication change. Such a bare review could become the breakthrough.
People also usually blame themselves because they believe that anxiety means weakness. It doesn’t. Anxiety means the stress system was overworked or overloaded. That system can be retrained.
The diagnostic journey
It is not a black and white test in diagnosis. It’s a back and forth chat plus if necessary, a quick check of the medical knowledge to rule out other stuff. Many of them feel nervous discussing it with a doctor, and the fear of fear is actual.
Mayo Clinic discusses using the GAD -7 as a standard screening test and research has demonstrated that the tool is fairly effective in identifying likely generalized anxiety disorder at standard cutoffs (typically quoted to be 80-90% sensitivity specificity by various settings).
Now, a typical pathway often looks like this:
- 🧾 Step 1: Symptom map — frequency, duration, triggers, and functional impact (sleep, work, relationships).
- 🩺 Step 2: Medical review — existing conditions, medicines, and substance use that could explain symptoms.
- 🧪 Step 3: Targeted testing — when appropriate, basic labs such as thyroid function, anemia screening, or other tests based on symptoms.
- 🧠 Step 4: Pattern diagnosis — distinguishing GAD vs panic disorder vs social anxiety vs phobias, and checking for related depression or trauma symptoms.
- 🧭 Step 5: Shared plan — therapy, medication, self-management steps, and follow-up cadence.
Another minor reason clinicians point out the difference is that most individuals refer to anxiety when it is actually panic or insomnia or a side effect of some medication. Determining the actual cause alters the course of treatment hence the significance of an appropriate diagnosis.
Treatment for Anxiety disorders
Treatment is not a cookie cutter prescription. When it is appropriate, the most prudent strategies combine abilities, self-control, and pharmacy. Progress is often somewhat stumbling along – two steps forward, one step backward. That’s normal.
According to Cleveland Clinic, many people respond to treatment, and evidence-based treatment such as CBT is the preferred treatment to most anxiety disorders. Most studies document significant improvement in a majority of patients who remain with regular care.
| Option | Best fit | What improvement can look like | Cost considerations | Common downsides |
|---|---|---|---|---|
| CBT (therapy) | Worry cycles, avoidance, panic patterns | Fewer symptoms, better coping, less avoidance | Session-based; coverage varies | Homework; discomfort during exposure practice |
| Exposure therapy | Phobias, social anxiety, panic avoidance | Triggers feel less dangerous over time | Often similar to CBT costs | Hard at first; requires consistency |
| SSRIs/SNRIs (medication) | Persistent anxiety, panic, comorbid depression | Lower baseline anxiety, fewer spikes | Generic options often affordable | Nausea, sleep changes, sexual side effects in some |
| Buspirone (medicine) | GAD-type symptoms for some patients | Gradual reduction in worry intensity | Often lower cost | Takes weeks; not for everyone |
| Short-term sedatives (selected cases) | Severe acute episodes when carefully monitored | Fast relief of intense symptoms | Usually inexpensive | Dependence risk, sedation, rebound anxiety |
| Lifestyle support (management) | All anxiety conditions as foundation | Better sleep, lower reactivity | Low cost | Needs routine; progress can be gradual |

Different treatments target different parts of the cycle: thoughts, behaviors, and body symptoms.
You see, though, you must take care of medicine. Some drugs can interact, some don’t play nice in pregnancy and some can wreak havoc when it comes to sleep initially. An exerciser will evaluate risks, benefits, side effects, and time of follow-up.
Therapy does not simply mean chatting. Good therapy is structured. The point is that it will use your brain to deal with any form of uncertainty and reduce the amount of avoidance.
Preventing Anxiety disorders and relapse
Prevention is not an ideal solution. It refers to the reduction of the stress load per day, thus there is less material to drive the symptoms. It is easy to be overwhelmed with a long list of tips, whereas a smaller repetitive list is more effective.
CDC suggests that adults should have 150 minutes of moderate-intensity exercises weekly, frequent movement is also consistently associated with improved mental state in the context of population research.
Daily (low-friction)
- Concrete sleeping and waking time as far as possible.
- Caffeine restricts itself to throwing your symptoms or sleep off.
- Practice of short breathing in order to reduce arousal.
Weekly (skills and exposure)
- Protected motor activities (number of walks).
- Little by little exposure to situations to avoid using coping mechanisms.
- One nurturing social touchpoint for alleviating isolation.
Monthly (maintenance)
- Review triggers and early warning indicators.
- Address any issues with the care team with meds and therapy objectives.
- Revive habits that are broken instead of having fresh beginnings.
Anxiety that is chronic is highly amplified by issues in sleep. A better sleep means easier and reduced symptoms, and risk of relapse reduces.
But relapse can still happen. It does not undo progress, but can be an indication of a stressor or a rest period in continual therapy skill or a disruption of continuity. A half-note Clegging up of the fiddle will avert a complete decline.
When to seek medical help
Some of the symptoms of anxiety overlap with heart, lung, endocrine, or neurological problems. The overlap is the reason why assessment is important particularly when symptoms are new, abrupt or extreme.
CDC still calls heart disease a top killer, so new chest pain should receive medical attention rather than be taken as a case of anxiety.
Safety signs: urgent vs routine
Urgent medical evaluation is required for chest pain that is associated with pressure, fainting, severe shortness of breath, development of a one-sided weakness, confusion or seizure.
Urgent mental health support is appropriate for thoughts of self-harm, inability to stay safe, or severe agitation. Regional crisis lines vary; in the United States, the 988 Lifeline is available.
Regular clinic treatment is suitable in cases of persistent symptoms of weeks, progressive symptoms, avoidance, and sleep and life interference.
And many cases land in the middle: not an emergency, but not something to ignore. Those cases often benefit most from early diagnosis and management.
Hania’s pattern: Hania had had a couple of weeks of tension, poor sleep and thoughts that refused to go away of what could have happened. The stress signs were physical – tight chest, nausea and shaky feeling while carrying out everyday tasks. Avoidance began small and it increased. So it was embarrassing, to be honest.
Johny’s turning point: Johny noticed the same symptoms and believed it was merely a stressful situation, but the relationship did not subside. CBT skills and gradual exposure were initiated after a health examination did not find any common health stuff. When I discussed side effects and timeframes with a physician, a low dose SSRI was later added. The life gradually returned to the usual days, and the harbingers could be distinguished in good time.
Yet, the optimistic aspect is uniform: when the nailed down cycle, the anxiety conditions are sensitive to organized care. People aren’t “broken.” They are in a cycle which can turn.
Latest research
Recent literature on anxiety disorders is concerned with access, personalization and measurement. That means increasing the amount of evidence-based therapy delivery, better matching medication to patients and better symptom tracking.
This is supported by the fact that thousands of mental health studies are listed on ClinicalTrials.gov, which is operated by NIH, and many of these are related to anxiety research.
- Large datasets (2023–2026):Institutions that are using biobank scale cohorts, ranging up to hundreds of thousands of people, study the correlation between sleep, markers of inflammation and the exposure to stress and their corresponding anxiety traits. These studies do not diagnose individuals but occurring Rivera risk factors.
- Digital CBT and blended care (2023–2026): Multi-sites programmes are experimenting on a massive scale with therapist-supported digital CBT with samples of often several hundred to well over a thousand. The useful goal would be to minimize wait times and make efficacy skill practice consistent between visits.
- Exposure support tools (2023–2026): Assisted exposure using VR and app-based exposure-assisted homework via controlled exposure trials, usually 100-400 are evaluated for better adherence. The mechanism is still exposure learning, the tools are intended to facilitate compliance.
And no, the advancement of research is not always in the form of a one miracle drug. It often involves the form that improved delivery of proven care imposed earlier, and fewer barriers.
Frequently asked questions
Stress and uncertainty are normal responses, which are anxiety. An anxiety disorder is diagnosed when the symptoms are not going away, they are hard to control and they lead to impairment. The clinicians determine duration, intensity, avoiding behaviors as well as disturbance of sleep or work or relationships. A diagnosis allows the treatment, therapy, and medication decisions to be customized in a safe way.
Yes. Nausea, diarrhea, abdominal pain, appetite changes, and “butterflies” can be part of the stress response. The gut and brain communicate through nerves and hormones, and anxiety can heighten gut sensitivity. Persistent GI symptoms still deserve evaluation, since other conditions can overlap.
Both can be effective, and the best choice depends on severity, diagnosis, safety factors, and access. Evidence-based therapy (especially CBT and exposure-based therapy) can change the anxiety cycle. Medication such as SSRIs or SNRIs can reduce baseline symptoms. Combination care is common, especially when symptoms are moderate to severe.
Therapy progress can begin within a few sessions when skills are practiced consistently, though full improvement may take longer. Many first-line medications take weeks to reach full effect. Early side effects can appear before benefits. Follow-up matters because dosage, therapy approach, and diagnosis refinement often improve outcomes.
Lifestyle changes can reduce relapse risk by lowering baseline arousal: consistent sleep routines, regular movement, reduced heavy caffeine use, and limiting alcohol misuse. Ongoing therapy skills like cognitive restructuring and gradual exposure are also protective. Lifestyle steps are supportive care, and severe anxiety may still need formal therapy and medication management.

💬 Share Your Experience
Share your thoughts, questions, or personal tips below. Our community and editorial team value respectful and insightful discussions.